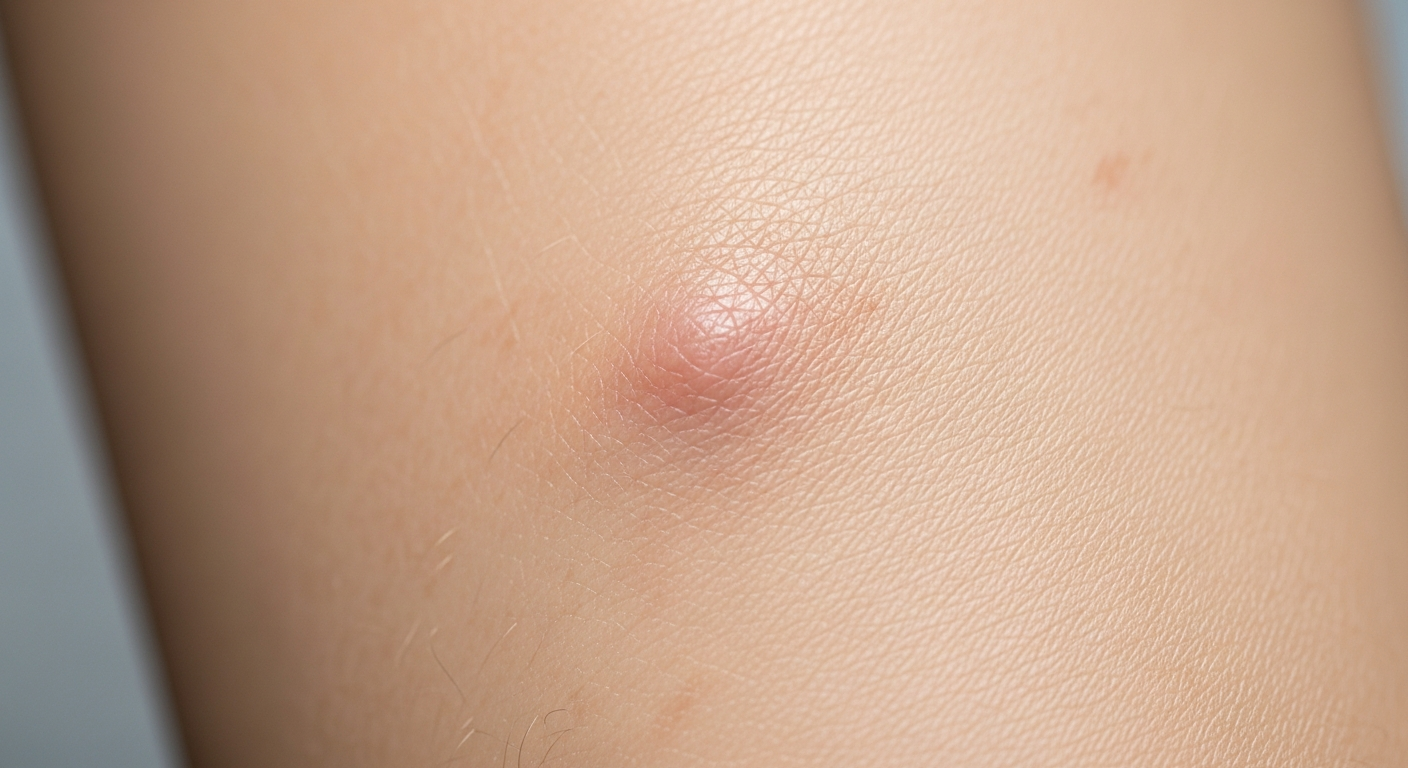
For a comprehensive understanding of this condition, examining Quincke’s edema symptoms pictures is crucial, as visual evidence often clarifies the subtle and overt manifestations. This article aims to provide detailed descriptions accompanying what one might observe in such images, focusing on the specific characteristics and locations of swelling associated with angioedema.
Quincke’s edema Symptoms Pictures
When reviewing Quincke’s edema symptoms pictures, one immediately observes the characteristic deep, localized swelling that defines this condition. Unlike superficial hives (urticaria), Quincke’s edema, also known as angioedema, affects the deeper layers of the skin and mucous membranes. This swelling is typically non-pitting, meaning it does not leave an indentation when pressed, and often presents with a firm, taut texture. The color of the affected skin can vary from normal skin tone to pale or, less commonly, erythematous (reddish), and it may feel warm to the touch. The onset of swelling is often rapid, developing within minutes to hours, and can be quite disfiguring, causing significant distress to the affected individual. The primary discomfort is usually a sensation of tightness, pressure, or burning rather than intense itching, which helps differentiate it from typical allergic rashes. In severe cases, pain may also be a prominent symptom, particularly when internal organs or joints are involved. The distribution of swelling is frequently asymmetrical, affecting one side of the face or a single limb more severely than the other. Understanding these visual cues is paramount for accurate recognition and prompt intervention.
The most common locations for visible Quincke’s edema symptoms include the face, particularly the lips, eyelids, and periorbital area. Swelling of the lips can make them appear grossly enlarged, protruded, and firm, often making speech and eating difficult. Eyelid swelling can be so severe that it obstructs vision entirely, causing the eyes to be swollen shut. The tongue can also swell dramatically, posing a significant risk to airway patency. Beyond the face, other frequently affected areas include the hands, feet, and genitalia. Swollen hands and feet can impede movement and daily activities, making it challenging to grasp objects or walk comfortably. Genital swelling, such as of the scrotum or labia, can cause considerable pain, discomfort, and embarrassment. While less commonly captured in Quincke’s edema symptoms pictures due to their internal nature, symptoms can extend to the gastrointestinal tract, leading to severe abdominal pain, nausea, vomiting, and diarrhea, mimicking acute abdominal emergencies. These internal manifestations can be just as debilitating and potentially life-threatening as external swelling. Therefore, a comprehensive assessment of all potential symptom locations is vital for diagnosis and management.
Key visible symptoms of Quincke’s edema include:
- Lip Swelling: Often dramatic and disfiguring, affecting one or both lips, making them appear thick, taut, and everted.
- Eyelid Swelling: Can be unilateral or bilateral, causing puffiness around the eyes, sometimes leading to complete closure of the eyelids and visual obstruction.
- Facial Swelling: General puffiness of the face, especially around the periorbital and perioral regions, often with a pale or slightly reddish hue.
- Tongue Swelling: Enlargement of the tongue, which can be visibly apparent, making speech difficult and posing a severe risk of airway obstruction.
- Hand Swelling: Diffuse swelling of the fingers and back of the hands, making them appear “sausage-like” and stiff, impairing dexterity.
- Foot Swelling: Similar to hand swelling, affecting the toes and top of the feet, making walking uncomfortable and fitting into shoes challenging.
- Genital Swelling: Pronounced swelling of the labia in females or scrotum in males, which can be painful and cause significant discomfort.
- Mucosal Swelling: While not always visible externally, swelling of the soft palate, uvula, and pharynx can be observed upon oral examination and is a critical warning sign for airway compromise.
- Abdominal Distension: Though not directly a skin symptom, severe internal edema of the bowel wall can lead to visible abdominal distension and tenderness, often mistaken for other abdominal pathologies.
- Skin Texture Changes: The skin over the swollen area may appear shiny, stretched, and smooth, often feeling firm and rubbery to the touch.
Signs of Quincke’s edema Pictures
Observing signs of Quincke’s edema pictures offers critical insights into the physical manifestations that clinicians and individuals need to recognize for timely intervention. The most striking sign is the rapid onset of localized swelling. This swelling typically appears as a well-demarcated, often asymmetrical, area of skin or mucous membrane involvement. For instance, a person experiencing this condition might exhibit a dramatically swollen upper lip while the lower lip remains relatively unaffected, or one eyelid might be significantly puffier than the other. The lack of associated itching is a distinguishing feature; instead, patients often report a sensation of burning, tightness, or pressure. This absence of pruritus helps differentiate angioedema from urticaria, which is characterized by intensely itchy wheals. The affected skin often appears normal in color, or slightly pale, though some individuals may present with a mild erythema. Importantly, the swelling is typically non-pitting, meaning that when pressure is applied to the swollen area, it does not leave a persistent indentation, unlike other forms of edema. This firmness to the touch is a consistent characteristic in Quincke’s edema pictures.
The progression of Quincke’s edema signs can be swift and alarming, particularly when vital areas such as the larynx are involved. Pictures showcasing laryngeal edema would reveal a person in acute respiratory distress, manifesting as stridor (a high-pitched whistling sound during breathing), hoarseness, difficulty swallowing (dysphagia), and shortness of breath (dyspnea). These are life-threatening signs that necessitate immediate medical attention. In such scenarios, the patient’s face might show signs of anxiety and struggle for air. Other less immediately life-threatening but significant signs include peripheral edema, such as profoundly swollen hands and feet. These areas might appear visibly distended, with the skin stretched taut and glossy. Pictures of such extremities would often show fingers and toes that resemble sausages, and the normal contours of the joints might be obscured by the swelling. Furthermore, involvement of the gastrointestinal tract, while not visible externally in pictures of the skin, can manifest as signs of severe abdominal pain, sometimes with distension or tenderness upon palpation, mirroring an acute surgical abdomen. These internal signs, if not recognized, can lead to misdiagnosis and inappropriate treatment. Therefore, a comprehensive understanding of both visible and reported signs is essential for managing Quincke’s edema effectively.
Specific observable signs that are crucial for identifying Quincke’s edema:
- Rapid Localized Swelling: The most obvious sign, appearing quickly in specific areas of the body.
- Asymmetry: Swelling often affects one side or one specific area more than others, creating an uneven appearance.
- Non-Pitting Edema: The swollen area remains firm and does not indent when pressed firmly, distinguishing it from typical fluid retention.
- Absence of Significant Itching: While some discomfort, burning, or tingling may be present, intense itching (pruritus) is typically absent, differentiating it from urticaria.
- Skin Discoloration: The skin over the edema may be normal-colored, pale, or mildly erythematous (reddish), often appearing stretched and shiny.
- Airway Compromise: Manifestations of laryngeal edema include:
- Stridor: A high-pitched, noisy breathing sound.
- Hoarseness: Changes in voice quality due to vocal cord swelling.
- Dysphagia: Difficulty or painful swallowing.
- Dyspnea: Shortness of breath, ranging from mild to severe, indicating airway obstruction.
- Cyanosis: A bluish discoloration of the skin and mucous membranes due to lack of oxygen (a late and very serious sign).
- Gastrointestinal Symptoms: Though not directly visible skin signs, severe abdominal pain, cramping, nausea, vomiting, and diarrhea can be accompanying signs of internal angioedema.
- Pain and Discomfort: Patients often report a sensation of pressure, tightness, or a burning pain in the affected areas.
- Functional Impairment: Swelling of joints (hands, feet) can limit movement and function, and facial swelling can impair speech and vision.
Early Quincke’s edema Photos
Examining early Quincke’s edema photos provides invaluable insight into the initial manifestations of this condition, which can sometimes be subtle and easily overlooked. The hallmark of early Quincke’s edema is its rapid onset, often evolving over minutes to a few hours rather than days. Initially, a person might experience a tingling, prickling, or burning sensation in a localized area before any visible swelling appears. This prodromal symptom can be a crucial warning sign. In the earliest stages, visible swelling may begin as a slight puffiness of the lips, eyelids, or a small patch of skin on the face or extremities. It might not be immediately alarming, often mistaken for a minor allergic reaction or a cosmetic issue. However, unlike typical allergic reactions which might start with itchy hives, early Quincke’s edema typically presents with a firm, localized, non-pitting swelling without significant itching. The skin overlying the swollen area may appear taut and smooth, often with normal color or a very subtle paleness, rather than a pronounced redness or rash. Recognizing these initial, less dramatic signs is critical for prompt diagnosis and intervention, especially given the potential for rapid progression to life-threatening scenarios.
Another key aspect in early Quincke’s edema photos is the potential for unilateral involvement. For instance, only one part of the lip might show slight enlargement, or one eyelid might begin to swell, giving an asymmetrical appearance. This initial asymmetry can be a distinguishing feature. As the condition progresses, the swelling can become more generalized within the affected region, but the rapid, localized characteristic remains. Early indications of laryngeal involvement are particularly important to identify. These might not be visually captured in typical photos but are described by patients as a feeling of throat tightness, a “lump in the throat,” or subtle changes in voice quality, such as hoarseness. These symptoms, even without obvious external neck swelling, signal an impending airway compromise and require urgent medical assessment. Similarly, early abdominal angioedema might present as mild, intermittent abdominal discomfort or bloating before progressing to severe pain. The absence of a widespread skin rash (urticaria) alongside these initial swelling manifestations is a strong indicator of isolated angioedema. Therefore, the ability to discern these specific early signs from more benign conditions is essential for effective patient care and preventing severe outcomes.
Key indicators to look for in early Quincke’s edema photos or during initial assessment:
- Subtle Localized Puffiness: The beginning of swelling may be slight, often affecting the periphery of the lips, corners of the eyes, or small areas of the hands or feet.
- Rapid Onset: The swelling appears quickly, usually within minutes to a few hours, rather than a gradual development over days.
- Tingling or Burning Sensation: Patients often report a preceding localized sensation of tingling, prickling, or mild burning before visible edema forms.
- Asymmetrical Presentation: Early swelling may affect only one side of a facial feature (e.g., one half of a lip) or one limb.
- Normal Skin Color or Pallor: The overlying skin may retain its normal color or appear slightly pale, contrasting with the redness seen in many allergic reactions.
- Lack of Intense Itching: Minimal to no itching, which helps differentiate it from the intensely pruritic wheals of urticaria.
- Firm, Non-Pitting Texture: Even in early stages, the swelling feels firm to the touch and does not leave an indentation upon pressure.
- Subtle Voice Changes: Early laryngeal involvement may manifest as a slightly hoarse voice, a “frog in the throat” sensation, or mild difficulty clearing the throat.
- Mild Throat Tightness: A feeling of constriction or a “lump” in the throat, indicating early swelling of the pharynx or larynx.
- Absence of Urticarial Rash: Pure angioedema typically presents without the accompanying red, itchy welts (hives) that characterize urticaria.
- Functional Impairment: Even minor swelling can lead to slight difficulty with speech, eating, or fine motor tasks, depending on the location.
Skin rash Quincke’s edema Images
It is important to clarify that Quincke’s edema, or angioedema, is fundamentally characterized by deep swelling of the dermis and subcutaneous or submucosal tissues, rather than a superficial skin rash in the typical sense of hives, macules, or papules. Therefore, when discussing skin rash Quincke’s edema images, it’s crucial to distinguish between pure angioedema and angioedema occurring concurrently with urticaria (hives). In cases of isolated angioedema, the skin over the swollen areas typically appears stretched, taut, and shiny. The color of the skin can range from normal skin tone to pale, or in some instances, mildly erythematous (reddish). However, there are usually no visible epidermal lesions, such as those associated with allergic rashes, eczema, or other dermatological conditions. The primary visual characteristic remains the localized, firm, non-pitting swelling. The sensation accompanying this swelling is usually one of tightness, pressure, or burning, with a notable absence of intense pruritus (itching). This distinction is vital for accurate diagnosis, as the presence or absence of a superficial rash guides the differential diagnosis and subsequent treatment strategies. Hence, images depicting pure Quincke’s edema would primarily show pronounced swelling without a concurrent visible rash on the skin’s surface.
When a “skin rash Quincke’s edema” scenario is depicted in images, it most commonly refers to the coexistence of angioedema with urticaria. Urticaria presents as distinct, intensely itchy, raised red wheals or hives that blanch with pressure and are typically migratory, appearing and disappearing within 24 hours in different locations. These hives affect the more superficial layers of the skin. If images show both deep swelling and these superficial itchy welts, it indicates an angioedema-urticaria syndrome, which often suggests an allergic mechanism. In contrast, forms of angioedema like hereditary angioedema (HAE) or acquired angioedema (AAE), which are bradykinin-mediated, very rarely present with urticaria. Therefore, images solely showing deep swelling without any accompanying rash are more characteristic of bradykinin-mediated angioedema. When examining skin rash Quincke’s edema images, one should focus on whether the rash is truly a superficial urticarial eruption or merely the taut, stretched appearance of skin overlying deep tissue swelling. Misinterpreting the skin’s appearance can lead to delays in appropriate, sometimes life-saving, treatment, especially in cases where the swelling involves critical areas like the airway. Understanding this distinction is fundamental for clinicians and patients trying to identify the condition.
Key characteristics of skin appearance in Quincke’s edema images, and its relation to a “rash”:
- Pure Angioedema (No Rash):
- Localized Swelling: The predominant visual finding is deep, often asymmetrical, swelling.
- Skin Texture: Overlying skin appears stretched, taut, and often shiny.
- Skin Color: Usually normal skin tone, pale, or mildly erythematous; not intensely red or inflamed like a typical rash.
- Lack of Epidermal Lesions: No papules, macules, vesicles, or typical “rash” elements are present on the skin’s surface.
- Non-Pitting: The swelling is firm and does not retain an indentation after pressure.
- Absence of Pruritus: Itching is minimal or absent, replaced by sensations of tightness, burning, or pressure.
- Angioedema with Urticaria (Associated Rash):
- Urticarial Wheals: Presence of distinct, raised, erythematous (red) or pale welts (hives) on the skin, which are intensely itchy.
- Migratory Nature: These wheals typically appear and fade within hours, often shifting locations.
- Superficial Involvement: Urticarial lesions affect the superficial dermis, unlike the deeper involvement of angioedema.
- Co-occurrence with Swelling: Both the deep swelling of angioedema and the superficial urticarial rash are visible simultaneously.
- Indicative of Allergic/Mast Cell Activation: This combination often points towards an underlying allergic reaction or mast cell activation.
- Important Distinctions:
- Not all angioedema presents with a rash. Bradykinin-mediated forms (HAE, AAE, ACEi-induced) rarely do.
- The “rash” in images should be carefully assessed to determine if it’s true urticaria or simply the visual effect of deeply swollen skin.
- Misidentification of a rash can lead to inappropriate treatment, especially in emergency situations where airway involvement is a risk.
Quincke’s edema Treatment
Quincke’s edema treatment is highly dependent on the underlying cause, the severity of the attack, and the location of the swelling. Given the potential for life-threatening airway obstruction, particularly with laryngeal involvement, emergency intervention is paramount. The immediate priority in all cases of significant angioedema is to secure the airway. This may involve intubation, cricothyrotomy, or tracheostomy in severe cases where swelling compromises breathing. Prompt recognition of respiratory distress, indicated by stridor, hoarseness, dysphonia, or dyspnea, is critical for timely intervention. Management strategies differ significantly between mast cell-mediated angioedema (often accompanied by urticaria and typically responsive to conventional allergy treatments) and bradykinin-mediated angioedema (such as hereditary angioedema, acquired angioedema, and ACE inhibitor-induced angioedema, which are generally unresponsive to antihistamines and corticosteroids).
For acute attacks of mast cell-mediated Quincke’s edema (often associated with allergies or idiopathic causes and frequently co-occurring with urticaria), the treatment protocol mirrors that for severe allergic reactions:
- Epinephrine: Administered subcutaneously, intramuscularly, or intravenously in cases of anaphylaxis or rapidly progressing airway compromise. It helps to reduce swelling and improve respiratory function.
- Antihistamines (H1 and H2 blockers): Intravenous diphenhydramine (H1 blocker) and ranitidine or cimetidine (H2 blockers) are often used to reduce histamine-mediated swelling and itching, especially if urticaria is present. Oral antihistamines may be used for milder attacks or as part of long-term management.
- Corticosteroids: Intravenous methylprednisolone or oral prednisone are used to reduce inflammation and prevent recurrence, especially for severe or persistent attacks. Their onset of action is slower, so they are not first-line for acute airway compromise.
- Fluid Resuscitation: Intravenous fluids may be necessary for patients experiencing hypotension or shock.
Bradykinin-mediated Quincke’s edema treatment, which includes Hereditary Angioedema (HAE), Acquired Angioedema (AAE), and ACE inhibitor-induced angioedema, requires specific therapies as it does not respond to epinephrine, antihistamines, or corticosteroids. These attacks are mediated by an excess of bradykinin, a vasodilator.
- For HAE and AAE acute attacks:
- C1-inhibitor (C1-INH) concentrate: Replaces the deficient or dysfunctional C1-INH protein, which regulates bradykinin production. Available as plasma-derived (e.g., Berinert, Cinryze, Ruconest) or recombinant (e.g., Rhucin) forms. This is often a first-line therapy.
- Icatibant (Firazyr): A bradykinin B2 receptor antagonist that blocks bradykinin from binding to its receptor, thereby preventing increased vascular permeability. Administered subcutaneously, often self-injectable.
- Ecallantide (Kalbitor): A kallikrein inhibitor that targets plasma kallikrein, an enzyme involved in bradykinin production. Administered subcutaneously.
- Fresh Frozen Plasma (FFP): Contains C1-INH and other plasma proteins, used as an alternative when specific C1-INH concentrates are unavailable, though it carries risks of infection and volume overload, and may paradoxically worsen some attacks.
- For ACE inhibitor-induced angioedema:
- Discontinuation of the ACE inhibitor: The primary and most crucial step.
- Airway Management: Aggressive airway management is paramount, similar to other forms of severe angioedema.
- Icatibant: Has shown effectiveness in accelerating resolution in some studies.
- C1-inhibitor concentrate: Evidence for its efficacy is still emerging, but it may be considered for severe or refractory cases.
- Fresh Frozen Plasma (FFP): Historically used, as it contains kininases that degrade bradykinin, but its effectiveness is debated and it carries risks.
Long-term prophylaxis for recurrent Quincke’s edema, particularly HAE, aims to reduce the frequency and severity of attacks:
- For HAE:
- Long-term C1-inhibitor concentrate: Regular intravenous infusions (e.g., Cinryze, Haegarda) to maintain adequate C1-INH levels.
- Attenuated Androgens: Such as Danazol or Stanozolol, which increase the synthesis of C1-INH in the liver. These are effective but have significant side effects, particularly in women and children.
- Lanadelumab (Takhzyro): A monoclonal antibody that inhibits plasma kallikrein, administered subcutaneously every 2-4 weeks. Highly effective in preventing HAE attacks.
- Berotralstat (Orladeyo): An oral plasma kallikrein inhibitor approved for HAE prophylaxis.
- Antifibrinolytics: Tranexamic acid or aminocaproic acid can be used for milder cases or as adjuncts, especially in children. They inhibit plasmin, which can activate the kallikrein-kinin system.
- For recurrent idiopathic angioedema without urticaria: Often treated with high-dose antihistamines and/or corticosteroids, with varying degrees of success. Immunosuppressants may be considered in refractory cases.
Trigger Avoidance and Patient Education:
A critical component of Quincke’s edema treatment is identifying and avoiding triggers. This includes:
- Medications: Avoiding ACE inhibitors, and in some cases, NSAIDs, can prevent drug-induced angioedema.
- Allergens: For allergic angioedema, strict avoidance of identified allergens is necessary.
- Physical Trauma/Stress: These can trigger attacks in some individuals, especially those with HAE.
- Infections: Viral or bacterial infections can sometimes precipitate attacks.
- Alcohol: Can be a trigger for some individuals.
Patients with a history of severe angioedema, especially HAE, should carry an emergency kit with their prescribed acute treatment medications and have a detailed emergency action plan. Education on recognizing early symptoms, administering self-injectable medications (like icatibant), and seeking immediate medical attention for signs of airway compromise is life-saving. Regular follow-up with specialists (allergists, immunologists) is essential for ongoing management and to adjust treatment strategies as needed. Psychological support can also be beneficial, as recurrent, unpredictable swelling can significantly impact quality of life.