When observing potential skin issues in young ones, understanding the precise presentation is crucial. This article provides an in-depth look at Urticaria in children symptoms pictures, offering detailed descriptions to aid in recognizing this common skin condition. We aim to equip parents and caregivers with comprehensive knowledge regarding the visual characteristics and associated signs of urticaria in pediatric populations.
Urticaria in children Symptoms Pictures
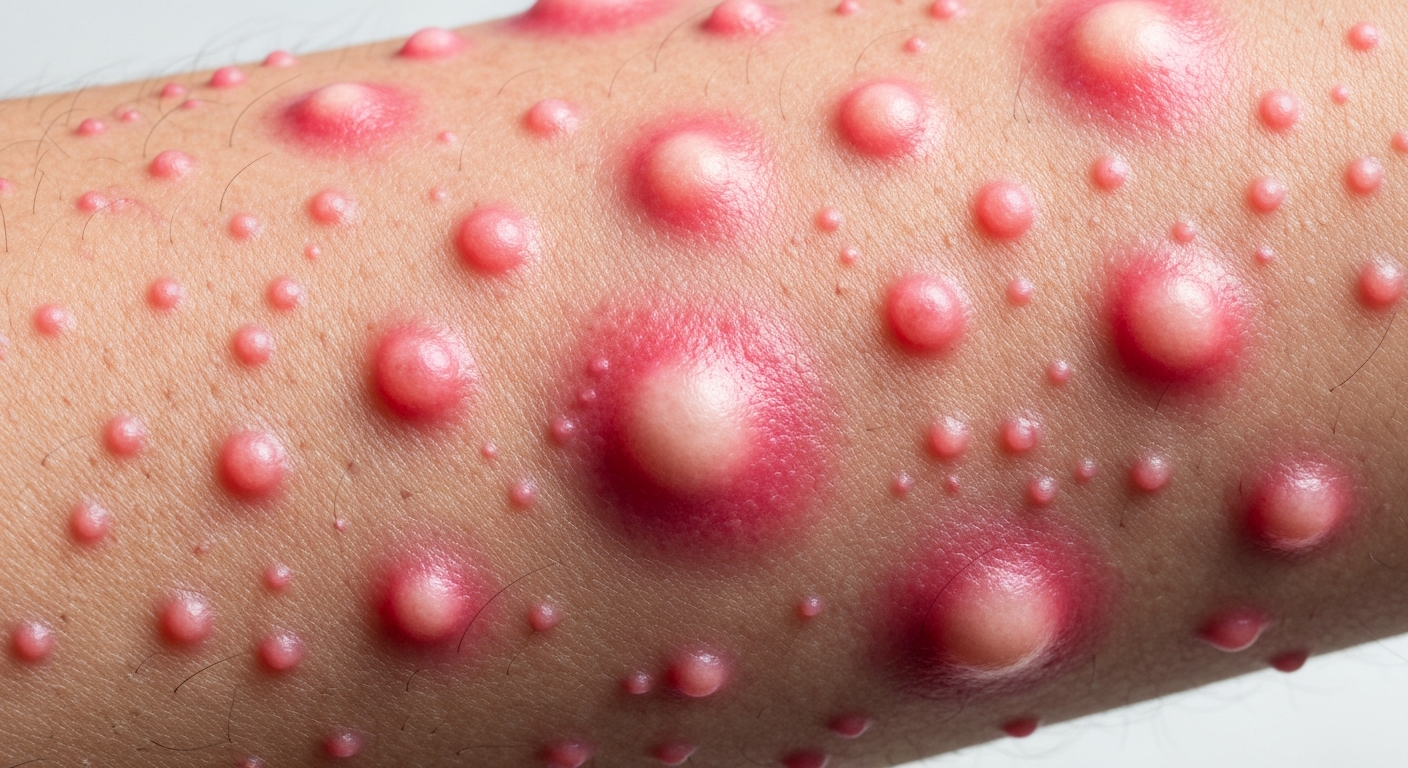
Identifying urticaria in children symptoms pictures involves recognizing the hallmark lesions known as wheals or hives. These are typically raised, itchy, red or pink bumps that appear on the skin. A key characteristic of urticarial lesions is their transient nature; they often appear quickly, last for minutes to a few hours, and then disappear, only to reappear in different locations. This migratory pattern is a strong indicator of urticaria. The size of these wheals can vary significantly, from tiny mosquito-bite-like bumps to large, confluent patches that cover extensive areas of the body. The intense pruritus, or itching, associated with these lesions can be very distressing for children, leading to sleep disturbances and irritability. Parents often describe the itch as relentless and maddening, prompting immediate investigation and relief strategies. The center of a wheal may sometimes appear paler than its periphery due to localized edema compressing capillaries, a phenomenon known as blanching. This visual detail can be helpful in distinguishing urticaria from other types of rashes.
The morphology of childhood urticaria symptoms can present in various ways, making a thorough visual assessment important. Here are some common symptomatic presentations:
- Individual Wheals: Discrete, circular or oval, elevated lesions with well-defined borders. These are the most classic representation and can range from a few millimeters to several centimeters in diameter.
- Confluent Plaques: Multiple individual wheals merging together to form larger, irregularly shaped, raised areas. These can cover significant portions of the trunk, limbs, or face, causing widespread discomfort.
- Annular Lesions: Wheals that clear in the center, forming ring-like patterns. This specific morphology can sometimes be mistaken for other dermatological conditions, but the transient and itchy nature helps differentiate it.
- Polycyclic Patterns: Multiple annular lesions that coalesce and overlap, creating complex, wavy or serpiginous (snake-like) patterns on the skin.
- Erythematous Patches: Areas of general redness underlying the wheals, particularly in cases where the wheals are numerous and densely packed. This diffuse redness is often a result of vasodilation in the surrounding skin.
- Pale Centers: A distinct pale or whitish area in the middle of a red wheal, indicative of central edema that pushes blood away from the superficial capillaries.
Common locations for hives in kids include almost any part of the body, but certain areas are frequently affected:
- Trunk: The chest, back, and abdomen are very common sites for widespread urticarial eruptions.
- Limbs: Arms and legs, including the hands and feet, can be extensively covered. Swelling of hands and feet can also occur as a form of angioedema.
- Face: Especially around the eyes and lips, which can also be indicative of angioedema, causing significant cosmetic distress and potential functional impairment if severe.
- Neck: Often affected, sometimes spreading from the trunk or face.
- Scalp: While less visible, itching on the scalp can be an indicator, sometimes accompanied by palpable small bumps.
- Buttocks: Frequently observed in younger children and infants, especially in contact urticaria cases.
Beyond the visible skin lesions, children with urticaria symptoms may exhibit other related discomforts:
- Intense Itching (Pruritus): The most common and often most debilitating symptom, leading to scratching, skin excoriations, and potential secondary infections.
- Burning Sensation: Some children describe a burning or stinging sensation accompanying the itch, particularly in areas with larger or more inflamed wheals.
- Generalized Discomfort: Feeling unwell, restless, or irritable due to persistent itching and lack of sleep.
- Sleep Disturbances: The nocturnal worsening of itch can severely disrupt sleep patterns for both the child and caregivers.
- Angioedema (Swelling): A deeper form of swelling that can affect the eyelids, lips, tongue, hands, feet, or genitalia. This is discussed in more detail under “Signs of Urticaria.”
- Difficulty Concentrating: Chronic itching can impact a child’s ability to focus on schoolwork or play.
It is paramount for parents to observe the duration of individual lesions. If lesions persist for more than 24 hours in a fixed location, it might suggest urticarial vasculitis or another underlying condition requiring a different diagnostic approach. However, classic pediatric urticaria is characterized by the fleeting nature of its lesions.
Signs of Urticaria in children Pictures
Beyond the primary wheals, several other signs of urticaria in children pictures can provide crucial diagnostic clues and indicate the severity or specific type of the condition. One significant sign is angioedema, which involves swelling of the deeper layers of the skin and subcutaneous tissues. Unlike superficial wheals, angioedema is often less itchy, but can cause a sensation of tightness, burning, or pain. It commonly affects the face (eyelids, lips, ears), hands, feet, and genitalia. When it affects the throat or tongue, it can be a medical emergency due to potential airway compromise, emphasizing the importance of prompt recognition and intervention for severe cases of childhood angioedema.
Another telling sign is dermatographism, sometimes referred to as “skin writing.” This phenomenon occurs when light stroking or scratching of the skin induces a localized wheal and flare reaction along the line of the stroke. It is a common form of physical urticaria and can be a definitive diagnostic marker for some children. The wheal typically appears within minutes of the stimulus and resolves within 30 to 60 minutes. Observing this specific reaction can help in understanding the underlying mechanisms of the child’s urticaria signs kids. The migratory nature of the lesions is also a key diagnostic feature: wheals appearing in one area, fading, and then reappearing in another site within hours. This transient and shifting pattern is a hallmark of typical urticaria, distinguishing it from static rashes.
Detailed examination of urticaria in children images should also focus on the following characteristic signs:
- Blanching: When pressure is applied to a wheal, its redness temporarily fades, and it appears pale or white. This indicates that the redness is due to superficial blood vessel dilation rather than hemorrhage into the skin. This differentiates urticarial lesions from purpuric rashes, which do not blanch.
- Perilesional Erythema: The redness extending slightly beyond the raised wheal itself, indicating a surrounding inflammatory reaction. This is a common finding and contributes to the overall red appearance of the affected area.
- Warmth to Touch: Affected skin areas, especially larger confluent plaques, may feel slightly warmer than the surrounding unaffected skin due to increased blood flow and localized inflammation.
- Deep-seated Swelling (Angioedema):
- Facial Swelling: Particularly around the eyes (periorbital edema) and lips (cheilitis). The lips can become markedly enlarged and everted.
- Laryngeal Edema: Swelling of the larynx and vocal cords, presenting as hoarseness, difficulty swallowing, or stridor. This is a medical emergency.
- Tongue Swelling: Macroglossia, where the tongue becomes significantly enlarged, potentially obstructing the airway.
- Extremity Swelling: Puffy hands and feet, which may make it difficult for the child to wear shoes or use their hands normally. This swelling is typically non-pitting.
- Genital Swelling: Swelling of the labia or scrotum, which can be alarming but is usually benign unless severe.
- Dermatographism:
- Mechanism: Triggered by mechanical trauma such as scratching, rubbing, or pressure.
- Appearance: A linear wheal (a raised, red welt) that forms precisely where the skin was stroked, often with a surrounding red flare.
- Timing: Develops within minutes and typically resolves within 30-60 minutes.
- Significance: Common in otherwise healthy individuals but more pronounced in children with chronic urticaria, offering a visible indicator of skin reactivity.
- Migratory Nature:
- Rapid Onset: Individual wheals appear suddenly.
- Quick Resolution: Most wheals resolve completely within 24 hours (often much sooner, within 2-4 hours).
- New Lesions: As old lesions fade, new ones appear in different body areas. This constant shift is characteristic.
In certain chronic forms of urticaria, particularly pressure urticaria, deeper, more painful swelling may occur in areas subjected to sustained pressure, such as from tight clothing or sitting. This type of reaction can manifest hours after the pressure has been applied, making it harder to link to a specific trigger. Observing whether the child has associated systemic symptoms, such as fever, joint pain, or gastrointestinal upset, is also important. While uncommon in typical pediatric urticaria, these symptoms could suggest a more complex underlying condition like urticarial vasculitis or an autoimmune disorder. The absence of fever and other systemic signs supports a diagnosis of simple urticaria.
Early Urticaria in children Photos
Recognizing early urticaria in children photos is critical for timely intervention and symptom management. The initial presentation of hives can often be subtle, starting as small, isolated, slightly reddish bumps that might be mistaken for insect bites or heat rash. However, a key differentiating factor is their rapid evolution: these initial bumps quickly enlarge, become more intensely red or pink, and develop the characteristic raised, edematous appearance of a wheal within minutes to a few hours. The intense itch often precedes or accompanies these early lesions, prompting the child to scratch, which can further aggravate the developing rash. Parents might first notice localized redness or a single itchy spot that then expands into a full-blown wheal. The transient nature means that by the time a doctor is seen, the “early” lesions might have faded, replaced by new ones, highlighting the utility of photographic documentation by parents.
The first few wheals often appear on areas of the body that have been exposed to a trigger, such as clothing friction, pressure, or contact with an allergen. For example, if a child is allergic to a particular fabric softener, the early lesions might appear first on the areas of skin that were in direct contact with the freshly laundered clothes. Similarly, a food allergen might lead to initial hives around the mouth or on the face before spreading. The rapid onset and progression from a subtle papule to a noticeable wheal within a short timeframe are strong indicators of acute urticaria early stage. Unlike many other skin rashes that develop slowly over days, urticaria manifests with striking speed, making its early recognition somewhat unique.
Key features to look for in first signs urticaria kids include:
- Small, Reddish Papules: The very first lesions may resemble small bug bites, typically 2-5 mm in diameter, slightly elevated, and red.
- Rapid Enlargement: These papules quickly expand outwards, often within 15-30 minutes, to form larger wheals.
- Intense Localized Itch: The child will likely complain of or demonstrate scratching at these early spots, even before they fully develop into classic wheals.
- Scattered Distribution: Initially, lesions may appear sparsely distributed before becoming more widespread.
- Warmth: The early affected areas may feel slightly warm to the touch.
- Indistinct Borders: Very early lesions might have less defined borders before the characteristic sharp demarcation of a wheal forms.
- Fleeting Nature: Even in their early stages, these lesions are transient. An early lesion seen on one part of the body might be completely gone an hour later, only for new ones to emerge elsewhere.
Factors that might trigger or exacerbate early hives children can include:
- Allergic Reactions:
- Food Allergens: Peanuts, tree nuts, milk, eggs, soy, wheat, fish, shellfish are common culprits. Reactions can be very rapid.
- Insect Bites/Stings: Localized or generalized hives can develop quickly.
- Medications: Antibiotics (especially penicillin), NSAIDs, and other drugs can trigger acute urticaria.
- Latex: Contact with latex products can cause immediate hives.
- Pet Dander/Pollen: Less common as a sole trigger for acute generalized urticaria but can exacerbate existing skin sensitivities.
- Infections:
- Viral Infections: Common colds, flu, mononucleosis, hepatitis, and other viral illnesses are frequent triggers, especially in young children.
- Bacterial Infections: Strep throat, urinary tract infections.
- Parasitic Infections: Less common in developed countries but can be a cause.
- Physical Stimuli:
- Pressure: From tight clothing, belts, or sitting.
- Temperature Changes: Cold (cold urticaria), heat (cholinergic urticaria), sun exposure (solar urticaria).
- Water: Aquagenic urticaria (rare).
- Vibration: Vibratory angioedema (rare).
- Stress/Emotional Factors: While not a direct trigger, emotional stress can lower the threshold for histamine release and exacerbate existing urticaria.
- Contactants: Certain plants (e.g., nettles), chemicals, or cosmetics coming into direct contact with the skin.
Observing the pattern of appearance and disappearance, coupled with the child’s reaction to the itch, helps confirm an early diagnosis of urticaria. Taking a photo of these initial lesions can be immensely helpful when consulting a healthcare provider, as the rash might have changed by the time of the appointment.
Skin rash Urticaria in children Images
The term “skin rash urticaria in children images” specifically refers to the collective appearance of wheals across a particular body area, emphasizing the generalized presentation that often occurs. Unlike many other childhood rashes that might be vesicular, maculopapular, or scaly, an urticarial rash is characterized by its distinct raised, edematous, and often erythematous nature. The “rash” aspect denotes the presence of multiple wheals, which can range from discrete and widely spaced to densely packed and confluent, creating large, irregular plaques. The color of the rash is predominantly red or pink, but as mentioned, individual wheals often have a paler center due to the localized fluid accumulation. This contrasting color can be a key visual identifier for urticarial rash kids.
The distribution of the hives rash children can vary, from localized eruptions due to contact or physical stimuli to generalized rashes covering most of the body in cases of systemic allergic reactions or infections. The texture of the rash is smooth and slightly taut when the skin is stretched, reflecting the underlying edema. It’s crucial to differentiate urticarial rashes from other common pediatric rashes, such as viral exanthems (which are typically non-itchy or mildly itchy and don’t blanch as readily), eczema (which is usually dry, scaly, and chronic), or insect bite reactions (which tend to be localized to exposed areas and don’t migrate as extensively). The rapid development and resolution of individual lesions remain the most distinctive characteristic, regardless of the overall pattern of the rash. A child presenting with a widespread, intensely itchy, migratory rash should immediately raise suspicion for urticaria.
Various patterns and characteristics define the itchy skin rash infants:
- Morphological Patterns of Urticarial Rashes:
- Discrete: Individual, well-separated wheals, common in initial stages or milder reactions.
- Confluent: Wheals merge to form large, irregularly shaped plaques. This often indicates a more severe or widespread reaction.
- Annular (Ring-shaped): Wheals with central clearing, forming rings.
- Arcuate (Arch-shaped): Curved or crescent-shaped wheals.
- Serpiginous (Snake-like): Wavy or meandering patterns formed by coalescing wheals.
- Targetoid: Rarely, urticarial lesions can appear somewhat like target lesions (concentric rings), which can be confused with erythema multiforme. However, true urticarial lesions are more transient and elevated.
- Color Characteristics:
- Bright Red/Pink: The most common coloration, indicating active inflammation and vasodilation.
- Pale Center: Due to localized edema compressing capillaries, a whitish or paler area is often seen in the center of the wheal.
- Erythematous Halo: A red flare surrounding the main wheal.
- Occasionally Darker Red/Purplish: In cases of urticarial vasculitis or severe inflammation, the color might be darker, and the lesions may be less transient. This requires medical evaluation.
- Texture and Feel:
- Smooth and Elevated: The surface of the wheal feels smooth, unlike the scaling of eczema or the roughness of some viral rashes.
- Tense/Edematous: The raised nature is due to fluid accumulation (edema) in the dermis.
- Warm to Touch: Due to increased blood flow.
- Non-pitting Swelling: Unlike typical edema (e.g., from heart failure), angioedema and urticarial wheals do not usually retain an indentation when pressed.
- Associated Symptoms within the Rash Area:
- Intense Pruritus: The hallmark symptom, often leading to excoriations from scratching.
- Burning/Stinging: Less common but can be reported, especially with larger lesions.
- Tenderness: If angioedema is present, the area might feel tender or painful rather than itchy.
When assessing rash urticaria in infants, it’s important to consider areas of vulnerability. Infants and young children often develop urticaria on the face, neck, and diaper area due to increased skin sensitivity and contact with potential irritants or allergens. For instance, new food introductions can lead to immediate perioral hives. The migratory nature means that the rash observed at one moment might be entirely different in distribution and intensity just a few hours later. Documentation through photographs at different stages can significantly aid in diagnosis and management, providing a visual timeline of the condition’s progression and regression. This photographic evidence helps track the efficacy of any given treatment or the identification of patterns related to triggers.
Urticaria in children Treatment
The treatment for urticaria in children primarily focuses on alleviating symptoms, identifying and avoiding triggers, and, in some cases, using medications to control the allergic response. The immediate goal is to reduce the intense itching and swelling to improve the child’s comfort and prevent secondary complications like skin infections from scratching. It’s crucial to emphasize that while this section outlines common treatments, all medical advice should be sought from a qualified healthcare professional. Self-medication or delayed medical attention, especially for severe cases with angioedema or breathing difficulties, can be dangerous.
The first line of therapy for most cases of childhood urticaria treatment involves antihistamines. These medications work by blocking histamine, a chemical released by the body during an allergic reaction, which is responsible for the itching and wheals. Second-generation antihistamines are generally preferred for children due to their lower sedative effects compared to first-generation options. For more severe or persistent cases, or those accompanied by significant angioedema, other medications may be considered.
Here’s a detailed breakdown of hives relief kids and treatment strategies:
- First-Line Pharmacological Treatments (Antihistamines):
- Second-Generation H1 Antihistamines: These are preferred due to their effectiveness and minimal sedation. They are taken daily to control symptoms.
- Cetirizine (Zyrtec): Commonly used, available over-the-counter, and suitable for infants from 6 months of age (under medical supervision for very young infants).
- Loratadine (Claritin): Another popular non-sedating option, also available OTC.
- Fexofenadine (Allegra): Effective and non-sedating.
- Desloratadine (Clarinex): A prescription option, active metabolite of loratadine.
- Levocetirizine (Xyzal): Prescription, active enantiomer of cetirizine, generally well-tolerated.
- First-Generation H1 Antihistamines: These can be used short-term, especially at night, due to their sedative effects which can help with sleep disruption caused by itching. However, they are generally avoided during the day due to drowsiness and other side effects.
- Diphenhydramine (Benadryl): Often used for acute relief, but causes significant drowsiness.
- Hydroxyzine (Atarax/Vistaril): Prescription only, potent antihistamine with sedative and anxiolytic properties.
- H2 Antihistamines (Adjunctive Therapy): Sometimes used in combination with H1 antihistamines for better symptom control, as H2 receptors are also involved in skin reactions.
- Famotidine (Pepcid): Current alternative, can be used off-label.
- Second-Generation H1 Antihistamines: These are preferred due to their effectiveness and minimal sedation. They are taken daily to control symptoms.
- Corticosteroids (Short-Term Use):
- Oral Corticosteroids (e.g., Prednisone): Reserved for severe acute urticaria or exacerbations of chronic urticaria that do not respond to antihistamines. They are used for a very short course (3-7 days) to minimize side effects. They rapidly reduce inflammation and swelling.
- Topical Corticosteroids: Generally not effective for urticaria as the pathology is deeper in the dermis, but may be used to relieve intense itching and inflammation from secondary excoriations.
- Emergency Treatment (for Anaphylaxis/Severe Angioedema):
- Epinephrine (Adrenaline): Administered via auto-injector (e.g., EpiPen) in cases of severe allergic reaction (anaphylaxis) with associated respiratory distress (difficulty breathing, wheezing, stridor) or rapid progression of angioedema, particularly involving the throat or tongue. Parents of children with known severe allergies should be trained on how to use an epinephrine auto-injector.
- Emergency Services: Immediate activation of emergency medical services (e.g., calling 911) is critical in these situations.
- Immunomodulatory Agents (for Chronic Urticaria not responding to antihistamines):
- Omalizumab (Xolair): A monoclonal antibody that targets IgE. Approved for chronic spontaneous urticaria in children 12 years and older (and increasingly used off-label in younger children under specialist guidance). Administered via subcutaneous injection.
- Cyclosporine: An immunosuppressant, used in severe, refractory cases under strict specialist supervision due to potential side effects.
Trigger Identification and Avoidance:
A crucial component of managing childhood urticaria is identifying and eliminating potential triggers, especially in acute cases. This involves careful observation and, sometimes, diagnostic testing.
- Food Diary: Keeping a detailed record of foods eaten and the timing of urticaria flare-ups can help pinpoint dietary triggers.
- Environmental Exposure Review: Assessing exposure to new pets, pollen, dust mites, or new cleaning products.
- Medication Review: Evaluating all medications, including over-the-counter drugs, supplements, and herbal remedies.
- Infection Screening: A doctor may order tests for underlying infections (e.g., strep throat, viral infections) if suspected.
- Physical Stimuli Avoidance: If physical urticaria is diagnosed (e.g., cold urticaria, dermatographism), advising the child to avoid specific triggers (e.g., cold water, tight clothing).
- Allergy Testing: Skin prick tests or specific IgE blood tests may be performed to identify food or environmental allergens, though often, urticaria is non-allergic or idiopathic.
Supportive Care and Home Remedies for Urticaria in children:
- Cool Compresses or Baths: Applying cool, damp cloths or taking a lukewarm bath (oatmeal baths can be soothing) can temporarily relieve itching. Avoid hot baths, which can worsen itching.
- Loose-fitting Clothing: Cotton, loose-fitting clothing reduces friction and irritation on the skin.
- Avoid Scratching: Keep fingernails trimmed short to prevent skin damage and secondary infections from scratching. Consider mittens for infants.
- Moisturizers: While not directly treating the urticaria, keeping the skin well-hydrated can help maintain skin barrier function and reduce general irritation. Fragrance-free options are best.
- Stress Management: Although not a direct cause, stress can exacerbate urticaria. Creating a calm environment and ensuring adequate rest can be beneficial.
- Hydration: Ensuring the child is well-hydrated is always good for overall health and skin integrity.
The prognosis for acute urticaria in children is generally excellent, with most cases resolving within weeks. Chronic urticaria, lasting more than six weeks, is more challenging but often manageable with ongoing treatment and diligent trigger avoidance. Regular follow-up with a pediatrician or a pediatric allergist/dermatologist is essential to tailor treatment plans and monitor for any underlying conditions. This comprehensive approach ensures that children with urticaria symptoms pictures receive the best possible care, leading to reduced discomfort and improved quality of life.