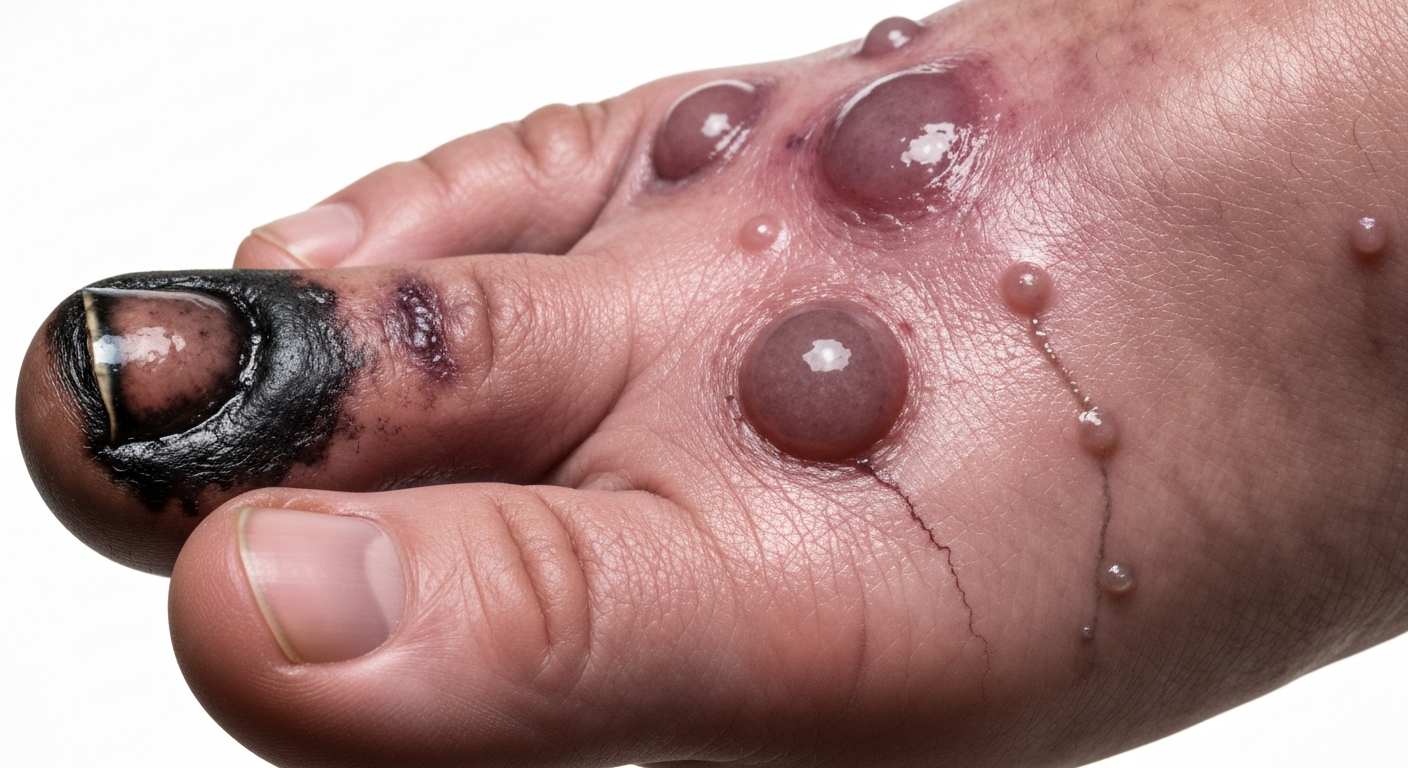
Recognizing the visual cues of various gangrene presentations is paramount for timely intervention and improved patient outcomes. This detailed guide offers an in-depth look at **Gangrene symptoms pictures**, focusing on the observable changes in affected tissues that demand immediate medical attention. Understanding these critical **signs of gangrene** can facilitate prompt diagnosis and lead to life-saving treatments.
Gangrene Symptoms Pictures
When examining **Gangrene symptoms pictures**, the visual identification of tissue death is critical. The appearance of gangrene varies significantly depending on its type, but common threads involve changes in skin color, texture, temperature, and the presence of associated discharge or systemic signs. These visual indicators are crucial for distinguishing gangrene from other skin conditions and for understanding the severity and progression of tissue necrosis.
Dry Gangrene Symptoms Pictures:
- Color Changes: The affected tissue, often an extremity like a toe or finger, typically appears shriveled and progresses through a spectrum of dark colors: from a pale blue or gray to a deep purplish-brown, eventually turning completely black. This striking discoloration is a hallmark of dry gangrene, resulting from a lack of blood flow rather than bacterial infection in its early stages.
- Texture: The skin becomes dry, brittle, and often leathery or mummified in appearance. It may feel cold to the touch and appear hardened or stiff. The lack of moisture due to ischemia contributes to this distinct, desiccated texture.
- Demarcation: A clear line of demarcation often forms between the healthy, living tissue and the dead, gangrenous tissue. This line can be sharp and distinct, making the extent of tissue damage visually apparent in **gangrene symptoms pictures**.
- Absence of Swelling or Pus: Typically, dry gangrene does not present with significant swelling, blistering, or a foul-smelling discharge unless secondary infection occurs. The absence of these features helps differentiate it from wet gangrene.
- Loss of Sensation: The affected area will often be numb due to nerve damage caused by prolonged lack of blood supply, though initial pain may be severe.
Wet Gangrene Symptoms Pictures:
- Swelling and Blistering: The affected area, which can include extremities or internal organs, appears swollen, moist, and often edematous. Blisters (bullae) filled with fluid, sometimes blood-tinged, are common and can rupture, leading to open, weeping sores.
- Skin Discoloration: The skin color rapidly progresses from red or mottled to a dusky reddish-brown, then purple, and eventually black. This discoloration is often irregular and spreads quickly, reflecting both tissue death and the presence of infection.
- Foul Odor: A distinguishing characteristic of wet gangrene is the strong, putrid, and foul odor emanating from the affected tissue. This odor is caused by the metabolic byproducts of bacterial decomposition.
- Pus and Discharge: There is often a significant amount of pus or other purulent discharge, which may be grayish, greenish, or dark brown. This discharge can be seen pooling around the necrotic tissue.
- Rapid Progression: Wet gangrene typically progresses much more rapidly than dry gangrene, spreading quickly through tissue planes due to the presence of bacterial infection and the moist environment.
- Systemic Symptoms: In addition to local signs, patients with wet gangrene often display systemic symptoms of infection, such as fever, chills, rapid heart rate (tachycardia), and low blood pressure (hypotension), indicating potential sepsis.
Gas Gangrene Symptoms Pictures:
- Rapid Discoloration: The skin over the affected muscle or tissue changes color very quickly, often within hours. Initial redness and tenderness can rapidly turn to a bronze, then reddish-purple, and finally a mottled black appearance.
- Crepitus: A unique and critical sign is crepitus, a crackling sensation felt or heard when the skin is palpated. This is caused by gas bubbles produced by the anaerobic bacteria (most commonly Clostridium perfringens) trapped within the tissues. This finding is often clearly visible in advanced **gas gangrene pictures** as distended, gas-filled areas under the skin.
- Blisters and Bullae: Large, tense blisters filled with brownish-red fluid (serosanguinous) are characteristic. These bullae may rupture, exuding a thin, watery, foul-smelling discharge.
- Severe Pain: Patients experience excruciating pain in the affected area, often disproportionate to the visible injury in its early stages.
- Foul Odor: A distinct sweetish, sickeningly foul odor, often described as “mousy” or “putrid,” is present due to bacterial fermentation.
- Rapid Spread: Gas gangrene is extremely aggressive, spreading with alarming speed and causing extensive tissue destruction, often leading to systemic toxicity and shock.
Internal Gangrene Symptoms Pictures:
While not visible in typical **gangrene symptoms pictures** of the skin, internal gangrene affects organs like the intestines, gallbladder, or appendix. Its signs are often systemic and indicative of severe infection:
- Severe, Localized Pain: Intense pain in the affected organ area (e.g., abdominal pain for intestinal gangrene).
- Fever and Chills: High fever is common due to systemic infection.
- Nausea and Vomiting: Often accompanied by a general feeling of being unwell.
- Low Blood Pressure: A sign of septic shock, especially in advanced cases.
- Peritonitis: If an internal organ ruptures, signs of peritonitis (abdominal rigidity, rebound tenderness) become apparent.
Fournier’s Gangrene Symptoms Pictures:
A specific type of wet gangrene affecting the perineum, genitals, or anal region, often seen in individuals with diabetes or compromised immune systems. Its **gangrene symptoms pictures** are striking:
- Rapidly Spreading Swelling and Erythema: Intense swelling, redness, and tenderness in the genital and perineal areas.
- Skin Discoloration: Rapid progression to dusky brown, purple, or black discoloration of the skin.
- Crepitus: Gas trapped under the skin is a common finding, indicating widespread infection.
- Foul Odor: A prominent, putrid odor due to polymicrobial infection.
- Blistering and Necrosis: Formation of blisters and rapidly spreading skin necrosis, leading to sloughing of affected skin.
- Severe Pain: Often presents with disproportionately severe pain.
Understanding these distinct visual characteristics from **gangrene symptoms pictures** is vital for rapid identification and intervention. Every type of gangrene represents a medical emergency requiring immediate attention.
Signs of Gangrene Pictures
Delving deeper into the observable **signs of gangrene pictures** provides a more granular understanding of the visual pathology. These signs are critical for healthcare professionals and anyone trying to understand the urgency of this condition. Early recognition of these specific visual cues can dramatically impact outcomes by facilitating prompt medical consultation.
Detailed Visual Signs from Gangrene Pictures:
- Skin Coloration Variations:
- Pale/Ashy Hue: Often an initial sign of arterial insufficiency, indicating reduced blood flow before complete tissue death. The skin may appear unusually pale or white, especially in dry gangrene.
- Mottling/Marbling: Irregular patches of discoloration, often purplish or reddish, resembling a marbled pattern. This indicates compromised microcirculation and is frequently seen in early wet gangrene.
- Reddish-Brown to Dark Purple: As tissue hypoxia worsens and blood stagnates, the hemoglobin deoxygenates, leading to darker discoloration. This is a common progression in both wet and dry gangrene.
- Black Eschar: The ultimate stage of necrosis, where the tissue becomes completely devoid of blood supply and appears hard, dry, and distinctly black. This is a definitive sign of advanced gangrene, particularly dry gangrene.
- Skin Texture Alterations:
- Dry and Shriveled: Characteristic of dry gangrene, where the lack of moisture causes the skin to shrink, wrinkle, and become brittle. It often resembles mummified tissue.
- Moist and Swollen: A key feature of wet gangrene, where infection leads to inflammation, fluid accumulation (edema), and a soft, boggy texture. The skin may appear stretched and shiny.
- Leathery or Hardened: In some forms of dry gangrene, the affected skin can become tough and leathery, almost like cured leather.
- Loss of Hair/Shiny Skin: In chronic arterial insufficiency leading to gangrene, the skin on the affected limb may become thin, shiny, and hairless due to poor nutrition and oxygenation.
- Presence of Blisters and Bullae:
- Fluid-Filled Blisters: Small to large vesicles or bullae (blisters) are frequently observed in wet gangrene and gas gangrene. These are indicative of severe tissue damage and fluid extravasation.
- Hemorrhagic Blisters: Blisters containing blood-tinged fluid are a more serious sign, often indicating deeper tissue necrosis and vascular compromise. These are particularly concerning in gas gangrene.
- Ruptured Blisters: Open, weeping sores resulting from ruptured blisters provide entry points for secondary infections and exude fluid or pus.
- Discharge and Odor:
- Purulent Discharge: Pus, often yellowish, greenish, or dark brown, is a clear sign of bacterial infection and is prevalent in wet and gas gangrene. Its presence denotes an active infectious process contributing to tissue destruction.
- Foul Odor: The strong, putrid smell associated with wet and gas gangrene is due to the anaerobic metabolism of bacteria. Descriptions range from “sweetish,” “mousy,” to “flesh-rotting,” and it’s an unmistakable sign in **signs of gangrene pictures** if smell could be conveyed.
- Gas Bubbles: Visible gas bubbles or frothy discharge can be present in gas gangrene, a direct result of bacterial gas production within the tissues.
- Temperature Changes:
- Cold to Touch: The affected area, especially in dry gangrene, often feels noticeably colder than surrounding healthy tissue due to the absence of blood flow.
- Warmth and Tenderness: In early wet gangrene or cellulitis preceding gangrene, the area may initially be warm, red, and exquisitely tender due to inflammation.
- Crepitus:
- Crackling Sensation: A distinctive sign of gas gangrene, felt as a crackling or crunching sensation when the skin is palpated. This indicates the presence of gas within the soft tissues. While not directly visible in **signs of gangrene pictures**, its effect (swelling, unusual texture) might be implied.
- Pain and Sensation Changes:
- Severe Pain: Often disproportionately severe, especially in gas gangrene or rapidly progressing wet gangrene.
- Numbness or Loss of Sensation: As nerves die due to lack of oxygen, the affected area can become numb, which can be deceptive as it may suggest a less serious condition.
- Pins and Needles: Early stages of ischemia might present with paresthesia (tingling or prickling sensation).
- Demarcation Line:
- Clear Separation: A distinct line or zone separating viable, healthy tissue from necrotic, dead tissue. This is a prominent feature in dry gangrene pictures. This line signifies the extent of irreversible damage.
Each of these visual **signs of gangrene pictures** contributes to a comprehensive diagnostic picture, guiding medical professionals toward the correct diagnosis and urgent management. The progression of these signs often dictates the urgency and type of intervention required.
Early Gangrene Photos
Identifying **Early Gangrene Photos** is critical because prompt intervention at this stage can often prevent more extensive tissue damage, reduce the need for amputation, and improve overall survival. The initial signs can be subtle and easily mistaken for less severe conditions, making keen observation essential. Recognizing these nascent changes often involves noticing subtle alterations in skin appearance, sensation, and local temperature before widespread necrosis sets in.
Early Signs of Dry Gangrene:
- Pallor or Cyanosis: The very first signs often include a noticeable paleness (pallor) of the skin, particularly in the digits, due to reduced blood flow. This might progress to a faint bluish tint (cyanosis) as oxygen saturation drops in the peripheral tissues. In **early gangrene photos**, this might appear as a slight grayish or purplish discoloration, often localized to the tips of fingers or toes.
- Coolness to Touch: The affected area will feel distinctly colder than the surrounding healthy skin. This difference in temperature is an early indicator of impaired circulation.
- Numbness or Tingling: Patients may report a sensation of pins and needles (paresthesia) or a gradual loss of sensation in the affected extremity, which is a neurological sign of ischemia.
- Intermittent Claudication: While not a direct skin sign, prior symptoms of pain in the leg muscles during exercise (claudication), which resolves with rest, is a strong precursor to dry gangrene and would be important context for **early gangrene photos** of a limb.
- Shiny, Thin Skin: Chronic lack of blood flow can cause the skin to become thin, atrophic, and shiny, often accompanied by loss of hair on the digits or foot. This isn’t gangrene itself but indicates severe peripheral arterial disease (PAD) that predisposes to it.
- Delayed Capillary Refill: When pressure is applied to the nail bed and released, the color return is noticeably slower than normal (greater than 2-3 seconds), indicating poor perfusion.
Early Signs of Wet Gangrene:
- Localized Redness and Swelling: Initial presentation often mimics cellulitis, with a spreading area of redness (erythema), warmth, and tenderness. However, the progression in wet gangrene is often more rapid and severe. **Early gangrene photos** might show an area of intense, angry-looking redness, potentially with slight induration.
- Pain Disproportionate to Injury: Patients may experience severe pain that seems out of proportion to the visible injury or infection. This is particularly true for gas gangrene precursors but applies to wet gangrene too.
- Small, Tense Blisters: The appearance of small, fluid-filled blisters (vesicles) or larger bullae on the inflamed skin. These might contain clear fluid initially but can quickly become hemorrhagic.
- Subtle Mottling or Marbling: Instead of uniform redness, the skin may begin to show a patchy, net-like, or mottled appearance, indicating microvascular compromise.
- Slight Foul Odor: While not as pronounced as in advanced wet gangrene, a subtle, unusual odor might be detectable in the very early stages, signaling bacterial activity.
- Increased Systemic Symptoms: Even in early stages, signs of systemic infection like low-grade fever, general malaise, or increased heart rate can be present, differentiating it from a localized, non-spreading infection.
Early Signs of Gas Gangrene:
- Sudden, Excruciating Pain: The onset is often marked by extremely severe, localized pain that intensifies rapidly and is far greater than what would be expected from the wound or injury. This is a hallmark early symptom.
- Rapid Swelling: The affected area, often around a surgical incision or deep wound, swells dramatically and quickly due to gas production and inflammation. **Early gangrene photos** would show an abnormally turgid and rapidly expanding limb.
- Bronze or Dusky Hue: The skin may initially turn a pale bronze or dusky color, often with a rapid progression to more ominous reddish-purple or gray patches.
- Early Crepitus: While sometimes subtle, a faint crackling sensation can be felt under the skin, especially at the wound edges, indicating the presence of gas. This is a critical early diagnostic sign.
- Blister Formation: Small, blood-filled bullae can form quickly over the affected area.
- Low-grade Fever and Tachycardia: Systemic signs of infection, such as a mild fever and an elevated heart rate, typically develop very rapidly.
Factors that Predispose to Early Gangrene:
- Diabetes Mellitus: Poorly controlled diabetes is a major risk factor, leading to neuropathy (loss of sensation) and peripheral arterial disease, making patients vulnerable to non-healing wounds that can progress to gangrene. **Early gangrene photos** of diabetic feet often show subtle changes around ulcers.
- Peripheral Arterial Disease (PAD): Any condition causing narrowing of arteries, such as atherosclerosis, severely reduces blood flow, predisposing to dry gangrene.
- Trauma or Surgery: Deep, penetrating wounds, crushing injuries, or certain surgeries can introduce bacteria deep into tissues, leading to wet or gas gangrene.
- Immunosuppression: Conditions like HIV/AIDS, cancer, or medications that suppress the immune system increase the risk of rapid infection progression.
- IV Drug Use: Can lead to localized infections and vascular damage, escalating to gangrene.
- Frostbite: Severe cold exposure causes tissue damage that can progress to dry gangrene. **Early gangrene photos** after frostbite might show initial waxy pallor, followed by blistering and then darkening.
The ability to interpret **early gangrene photos** and recognize these initial, often subtle, visual and symptomatic changes is paramount. Delay in diagnosis even by a few hours can significantly worsen the prognosis, emphasizing the urgency of medical evaluation when any of these signs are observed.
Skin rash Gangrene Images
While gangrene is fundamentally tissue necrosis, certain conditions can manifest with “skin rash” like appearances that rapidly progress to gangrene, or are direct precursors. These **Skin rash Gangrene Images** highlight instances where seemingly benign skin changes can quickly escalate into severe necrotic processes, demanding a high index of suspicion. It is crucial to differentiate these serious presentations from common dermatological rashes, as misdiagnosis can have catastrophic consequences.
Conditions with Rash-like Presentations Leading to Gangrene:
- Ecthyma Gangrenosum:
- Appearance: Typically starts as a painless, reddish-purple macule or papule, often surrounded by an erythematous halo. Within hours to days, it rapidly progresses to a hemorrhagic bulla (blood-filled blister), which then ruptures to form a necrotic ulcer with a distinctive black eschar (scab) and undermined edges.
- Causative Agent: Most commonly associated with Pseudomonas aeruginosa infection in immunocompromised individuals, but can also be caused by other bacteria.
- Location: Can occur anywhere on the body, but common sites include the axilla, anogenital area, and extremities. **Skin rash Gangrene Images** of ecthyma gangrenosum show these rapid, destructive lesions.
- Progression: The speed of progression from a small ‘rash’ to a deep necrotic ulcer is the key differentiator.
- Purpura Fulminans:
- Appearance: Characterized by acute onset of rapidly progressive, symmetrical skin necrosis accompanied by disseminated intravascular coagulation (DIC). It begins with erythematous macules that quickly evolve into ecchymoses (large bruises) and purpuric patches that are painful and often have irregular, jagged borders. These lesions then progress to hemorrhagic bullae and full-thickness skin necrosis with black eschar.
- Causative Agents: Often triggered by severe infections (e.g., meningococcemia, streptococcal toxic shock syndrome) or other severe inflammatory states.
- Location: Commonly affects the extremities, buttocks, and trunk. **Skin rash Gangrene Images** of purpura fulminans are often dramatic, showing widespread, dark, necrotic patches.
- Pathophysiology: Involves widespread thrombosis (blood clot formation) in small and medium-sized blood vessels of the skin.
- Warfarin-Induced Skin Necrosis:
- Appearance: Typically develops within a few days of starting warfarin therapy. It begins as painful, erythematous, and edematous plaques that progress to purpuric patches, hemorrhagic bullae, and eventually full-thickness skin necrosis with sharply demarcated borders.
- Mechanism: Due to a transient hypercoagulable state caused by the rapid depletion of protein C (an anticoagulant) relative to procoagulant factors during initial warfarin therapy, leading to microvascular thrombosis.
- Location: Commonly affects areas with abundant subcutaneous fat, such as breasts, thighs, buttocks, and abdomen. **Skin rash Gangrene Images** would show these distinct areas of necrosis.
- Calciphylaxis (Calcific Uremic Arteriolopathy):
- Appearance: Characterized by intensely painful, violaceous (purplish) skin lesions, often resembling livedo reticularis initially, that progress to ulcers with a necrotic black eschar. These lesions are excruciatingly painful and often non-healing.
- Associated Conditions: Primarily seen in patients with end-stage renal disease, hyperparathyroidism, and obesity.
- Mechanism: Involves calcification of small and medium-sized arteries in the dermis and subcutaneous fat, leading to ischemia and necrosis.
- Location: Most common on the lower extremities, abdomen, and buttocks. The rash-like initial presentation evolves into severe gangrenous ulcers, clearly depicted in **Skin rash Gangrene Images**.
- Atheroembolic Disease (Cholesterol Embolism):
- Appearance: Can manifest as livedo reticularis (a net-like purplish discoloration), ‘blue toe syndrome’ (bluish discoloration of toes without pain), or patchy areas of necrosis, resembling a rash or mottled skin initially.
- Mechanism: Embolization of cholesterol crystals and other debris from proximal atherosclerotic plaques (e.g., in the aorta) into smaller peripheral arteries, leading to microvascular occlusion and ischemia.
- Progression: While not always leading to frank gangrene, these ‘rash’ like appearances signify severe vascular compromise and can progress to digital or localized necrosis.
- Severe Cellulitis with Impending Necrosis:
- Appearance: While cellulitis itself is an infection of the deeper layers of skin, in severe cases, particularly with aggressive bacterial strains (e.g., necrotizing fasciitis precursor), the overlying skin can develop rapid changes. This might include rapidly spreading erythema that darkens, becomes violaceous, forms bullae, and shows signs of impending necrosis, moving beyond a typical ‘rash’ to a pre-gangrenous state.
The key takeaway from studying **Skin rash Gangrene Images** is the recognition of rapid progression, disproportionate pain, and the evolution of seemingly superficial skin lesions into deep, necrotic ulcers. Any ‘rash’ or skin lesion that is exquisitely painful, rapidly spreading, discolored, or associated with systemic signs of illness (fever, shock) warrants immediate and thorough medical evaluation to rule out gangrene or a condition predisposing to it. Prompt diagnosis and intervention are critical in these high-stakes scenarios.
Gangrene Treatment
Effective **gangrene treatment** is an urgent, multi-faceted approach focused on halting the progression of tissue necrosis, controlling infection, managing underlying causes, and preserving as much healthy tissue and function as possible. The specific treatment modalities depend heavily on the type of gangrene, its extent, and the patient’s overall health. Early diagnosis is paramount for maximizing the chances of successful intervention and preventing life-threatening complications.
Immediate Medical Interventions:
- Surgical Debridement:
- Goal: The cornerstone of gangrene treatment is the prompt surgical removal of all dead, necrotic tissue. This procedure, known as debridement, is critical to stop the spread of infection, remove the source of toxins, and expose healthy tissue for healing.
- Extent: Can range from a minor local debridement to extensive tissue excision, sometimes requiring repeat surgeries (staged debridement) until all non-viable tissue is removed.
- Amputation: In severe cases, especially with extensive tissue death, uncontrollable infection, or if a limb becomes non-functional, amputation of the affected digit, limb, or part of an internal organ may be necessary to save the patient’s life and prevent further spread.
- Antibiotic Therapy:
- Indication: Essential for wet gangrene, gas gangrene, and any form of gangrene with signs of bacterial infection or sepsis.
- Administration: Typically administered intravenously, often with broad-spectrum antibiotics initially, which may be narrowed down once bacterial cultures and sensitivities are known.
- Duration: Treatment can be prolonged, lasting for weeks, depending on the severity of the infection.
- Hyperbaric Oxygen Therapy (HBOT):
- Mechanism: Involves breathing 100% oxygen at increased atmospheric pressure in a specialized chamber. This significantly increases the amount of oxygen dissolved in the blood and delivered to tissues.
- Benefits:
- Inhibits Anaerobic Bacteria: Highly effective against anaerobic bacteria (like Clostridium perfringens in gas gangrene) which thrive in low-oxygen environments.
- Promotes Healing: Stimulates angiogenesis (formation of new blood vessels) and enhances the activity of white blood cells to fight infection.
- Reduces Swelling: Helps reduce tissue edema, especially in ischemic conditions.
- Indications: Particularly valuable for gas gangrene, severe necrotizing soft tissue infections, and certain non-healing wounds where oxygen delivery is compromised.
- Vascular Surgery/Intervention:
- Revascularization: For dry gangrene caused by severe peripheral arterial disease (PAD), procedures to restore blood flow to the affected limb are crucial.
- Angioplasty and Stenting: Minimally invasive procedures to open blocked or narrowed arteries using balloons and/or stents.
- Bypass Surgery: A surgical procedure to create a new path for blood flow around a blocked artery using a graft (either a vein from the patient’s body or a synthetic tube).
- Thrombolysis/Embolectomy: Procedures to dissolve or surgically remove blood clots that are blocking arteries.
- Goal: Improving blood supply to the ischemic tissue can prevent further tissue death, promote healing of remaining viable tissue, and potentially avoid amputation.
Supportive Care and Management of Underlying Conditions:
- Pain Management: Gangrene, especially wet and gas gangrene, is extremely painful. Aggressive pain control with strong analgesics is essential for patient comfort.
- Fluid and Electrolyte Management: Patients with severe infections and tissue loss can become dehydrated and have electrolyte imbalances, requiring intravenous fluid administration.
- Nutritional Support: Adequate nutrition is vital for wound healing and overall recovery, especially for patients undergoing extensive surgeries or with chronic conditions.
- Diabetes Control: For diabetic patients, strict control of blood glucose levels is paramount, as hyperglycemia impairs immune function and wound healing, contributing to gangrene progression.
- Smoking Cessation: Smoking severely impairs circulation and oxygen delivery, making it a critical factor to address in patients with peripheral arterial disease and gangrene.
- Wound Care: After debridement, meticulous wound care, including appropriate dressings, negative pressure wound therapy (NPWT), and regular cleaning, is necessary to promote granulation and epithelization.
- Monitoring for Sepsis: Close monitoring for signs of systemic infection (sepsis, septic shock) is critical. This includes monitoring vital signs, blood tests, and mental status.
- Rehabilitation: Following extensive surgeries or amputations, physical and occupational therapy are vital for regaining mobility and adapting to new physical challenges.
The **gangrene treatment** pathway is highly individualized and often involves a multidisciplinary team, including surgeons (vascular, general, orthopedic), infectious disease specialists, critical care physicians, wound care nurses, and rehabilitation therapists. The overarching goal is not just to treat the visible symptoms but to address the root causes and prevent recurrence, underscoring the severity and complexity of this life-threatening condition.