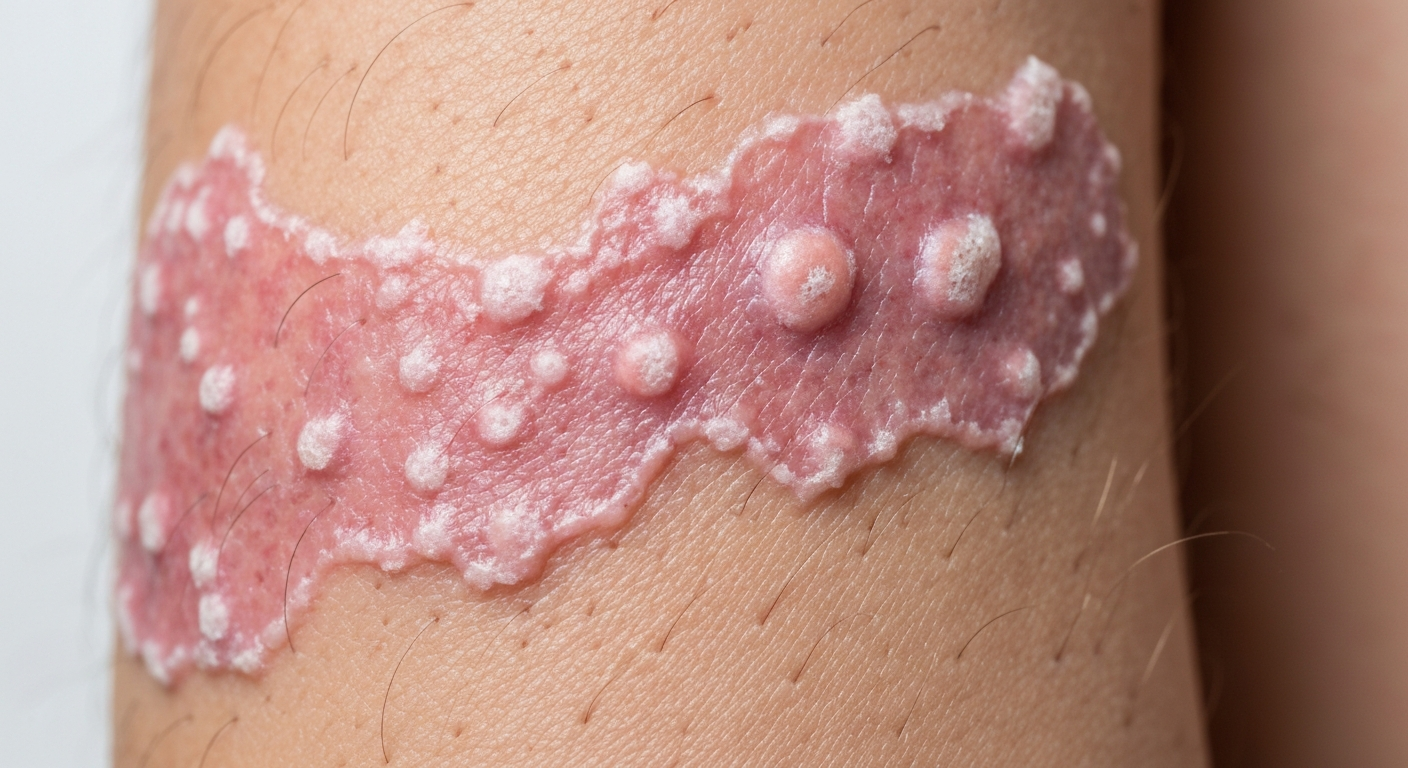
This detailed resource provides an in-depth look at various presentations of Erythema symptoms pictures, offering comprehensive descriptions for better understanding. Our aim is to illustrate the diverse visual characteristics associated with different forms of erythema, aiding in identification and awareness. Through a focus on observable signs and patterns, this guide serves to delineate the manifold ways erythema manifests on the skin.
Erythema Symptoms Pictures
Erythema, or redness of the skin, is a fundamental sign of inflammation, infection, or irritation. Observing the specific visual characteristics of erythema is crucial for proper dermatological assessment. When examining Erythema symptoms pictures, dermatologists and patients alike look for distinct patterns, colors, and associated features that can point to an underlying condition. The intensity of redness can vary from a faint pink blush to a deep, fiery crimson, often accompanied by warmth to the touch, swelling, and sometimes pain or itching.
The morphology and distribution of erythema provide significant diagnostic clues. For instance, some forms of erythema present as diffuse, widespread redness, while others are sharply circumscribed or follow specific anatomical patterns. Understanding these variations in erythema symptoms is paramount for accurate identification. Visual inspection focuses on several key attributes:
- Color intensity and shade: Ranging from pale pink to intense red, purple, or even bluish hues depending on the depth and cause of inflammation and the patient’s skin tone. Darker skin tones may present with hyperpigmentation, appearing as darker brown or purplish patches rather than classic red.
- Blanching: Determining if the redness disappears temporarily when pressure is applied (blanching) or if it remains unchanged (non-blanching purpura). Blanching indicates capillary dilation, while non-blanching suggests extravasation of blood into the tissue.
- Location and distribution: Whether the erythema is localized to a small area, generalized over large body surfaces, or affects specific regions like the face, extremities, or trunk. Patterns can be symmetrical or asymmetrical.
- Shape and borders: Lesions can be round, oval, linear, annular (ring-shaped), serpiginous (wavy or snake-like), arcuate (arc-shaped), or reticulated (net-like). Borders can be sharply defined, irregular, or poorly demarcated.
- Associated surface changes: The presence of scaling, crusting, vesicles (small blisters), bullae (large blisters), pustules (pus-filled lesions), erosions, ulcers, or lichenification (thickening of the skin).
- Palpation: Assessing if the area is warm, tender, indurated (hardened), or edematous (swollen).
Let us delve into specific types of erythema and their characteristic visual symptoms often captured in erythema pictures:
- Erythema Multiforme (EM): This condition is recognized by its classic “target” or “iris” lesions, which are often described as three concentric rings of color: a central dark area (sometimes blistered or crusted), surrounded by a pale edematous ring, which is then encircled by an outer red halo. These lesions frequently appear on the palms, soles, and extensor surfaces of the extremities, and may also involve mucous membranes, leading to painful erosions in the mouth, eyes, or genitals.
- Erythema Nodosum (EN): Characterized by tender, warm, red to purplish nodules, typically found on the shins, but occasionally on the thighs, forearms, or other areas. These lesions evolve over several weeks, often changing color much like a bruise, from red to purple, then brownish-yellow, before resolving without scarring. The symmetry and deep-seated nature of these subcutaneous nodules are key visual identifiers in Erythema Nodosum pictures.
- Erythema Migrans: The hallmark rash of early Lyme disease, this lesion begins as a small red macule or papule at the site of a tick bite and gradually expands outwards over days to weeks, forming an annular or “bullseye” appearance with central clearing. The lesion is often warm to the touch and may be asymptomatic or mildly itchy/painful. Its expanding nature is a critical visual sign in Lyme disease erythema pictures.
- Erythema Annulare Centrifugum (EAC): This persistent, chronic eruption presents as slowly enlarging, ring-shaped (annular) or arcuate erythematous plaques with a characteristic trailing scale on the inner edge of the advancing border. The central area often clears, leaving a slightly hyperpigmented or normal-looking center. These lesions can be solitary or multiple and are most commonly found on the trunk and proximal extremities.
- Erythema Toxicum Neonatorum: A common benign rash in newborns, visually identified by blotchy red macules (flat spots) and papules (raised bumps) that often develop into pustules (pus-filled bumps) or vesicles (small blisters) on an erythematous base. It typically appears on the face, trunk, and proximal extremities within the first few days of life, sparing the palms and soles.
- Erythema Ab Igne: This distinctive reticulated, net-like, or lace-like pattern of redness and hyperpigmentation results from prolonged or repeated exposure to moderate heat without burning. It often occurs on the shins (from heating pads or prolonged sitting near fires), back (laptop use), or abdomen (hot water bottles). The pattern mirrors the heat source and is typically non-blanching.
- Solar Erythema (Sunburn): A common form of erythema presenting as diffuse, often sharply demarcated redness of skin exposed to ultraviolet radiation. Depending on severity, it can range from mild pinkness to intense red with tenderness, warmth, swelling, and blistering. Later, scaling and peeling often occur.
- Erythema Chronicum Migrans: While often synonymous with Erythema Migrans, sometimes this term is used to emphasize the chronic and migratory nature of the lesion in untreated Lyme disease, where the rash can persist for weeks or months.
- Erythema Elevatum Diutinum (EED): A rare, chronic skin condition characterized by persistent, symmetrical, red-to-brownish-purple papules, plaques, and nodules, predominantly affecting the extensor surfaces of joints (e.g., elbows, knees, ankles, hands, feet). The lesions are often firm and can be asymptomatic or mildly pruritic or painful.
- Erythema Induratum (Bazin’s Disease): Visually presents as deep, tender, bluish-red subcutaneous nodules and plaques, most commonly on the calves of women, often bilateral. These lesions may ulcerate and heal with atrophic scars.
- Erythema Pernio (Chilblains): Characterized by localized redness, swelling, itching, burning, and sometimes blistering of the skin, typically on the fingers, toes, ears, and nose, appearing several hours after exposure to cold, non-freezing temperatures. The lesions are often purplish-red and resolve spontaneously within 1-3 weeks if further cold exposure is avoided.
- Rosacea: A chronic inflammatory skin condition primarily affecting the face, visually identifiable by persistent facial redness (erythema), flushing, telangiectasias (visible blood vessels), papules, and pustules. It typically spares the perioral and periocular areas (unlike perioral dermatitis).
- Contact Dermatitis: Presents as localized redness, swelling, vesicles, papules, and intense itching at the site of contact with an allergen or irritant. The shape and distribution of the rash often mirror the shape of the offending agent, making contact dermatitis pictures highly distinctive.
- Cellulitis: A bacterial skin infection causing a rapidly spreading, warm, tender, and intensely red area of skin, often with poorly defined borders. The erythema associated with cellulitis can quickly enlarge and may be accompanied by fever and chills.
- Urticaria (Hives): Characterized by transient, intensely itchy wheals (raised, red or pale bumps) that blanch with pressure and can appear anywhere on the body. Individual lesions typically resolve within 24 hours but new lesions may continuously appear.
Careful observation of these descriptive features in erythema symptoms pictures allows for a more refined diagnosis and appropriate management plan, emphasizing the critical role of visual analysis in dermatology.
Signs of Erythema Pictures
Understanding the observable signs of erythema goes beyond mere redness; it involves discerning the specific characteristics that contribute to a diagnosis. When examining Signs of Erythema Pictures, one is looking for objective, verifiable changes in the skin’s appearance, texture, and configuration. These signs are often categorized by their morphology, distribution, and associated features, which together paint a clearer clinical picture.
The primary signs of erythema are related to the vasodilation of blood vessels in the skin, leading to increased blood flow and the characteristic red appearance. However, the manifestation of this redness can vary significantly. Key observable signs include:
- Macules: Flat, discolored spots, typically less than 1 cm in diameter. Erythematous macules are simply flat areas of redness. They are common in conditions like drug eruptions (morbilliform rash) or viral exanthems.
- Patches: Larger flat areas of discoloration, greater than 1 cm. Erythematous patches are extensive flat areas of redness, such as those seen in severe sunburn or some forms of contact dermatitis.
- Papules: Small, raised, solid bumps, typically less than 1 cm in diameter. Erythematous papules are red, raised lesions, often found in conditions like insect bites, folliculitis, or acne.
- Plaques: Broad, raised, flat-topped lesions, greater than 1 cm, formed by the confluence of papules or by a larger area of induration. Erythematous plaques are characteristic of psoriasis (often with silvery scales), chronic eczema, or some forms of lupus.
- Nodules: Deeper, palpable, solid lesions, often greater than 1 cm, extending into the dermis or subcutaneous tissue. Erythematous nodules are typically warm and tender, as seen in erythema nodosum or deep infections.
- Wheals (Hives): Transient, elevated, compressible, itchy lesions with central pallor and surrounding erythema. They are the defining sign of urticaria and appear and disappear rapidly.
- Vesicles: Small, fluid-filled blisters, typically less than 0.5 cm. Erythematous vesicles are common in herpes simplex, herpes zoster, chickenpox, or acute contact dermatitis.
- Bullae: Large, fluid-filled blisters, greater than 0.5 cm. Erythematous bullae indicate more severe inflammation or conditions like bullous impetigo or bullous pemphigoid.
- Pustules: Small, pus-filled lesions. Erythematous pustules are often seen in acne, folliculitis, or pustular psoriasis.
- Scales: Flaky layers of stratum corneum, indicating increased epidermal turnover or impaired desquamation. Erythematous lesions with scales are classic signs of psoriasis, seborrheic dermatitis, or fungal infections.
- Crusts: Dried serum, blood, or pus on the skin surface. Erythematous lesions can become crusted after vesicles or pustules rupture, common in impetigo or herpes lesions.
- Erosions: Superficial breaks in the epidermis that do not extend into the dermis, often resulting from ruptured vesicles or scratching.
- Ulcers: Deeper breaks in the skin, extending into the dermis or subcutaneous tissue, which can be seen with chronic inflammation or infection, often with surrounding erythema.
- Purpura: Non-blanching red or purple discolorations due to extravasation of blood into the skin. When palpable (raised), it is a significant sign of vasculitis, an inflammatory condition of blood vessels.
In signs of erythema pictures, the pattern of distribution is also highly indicative. Examples include:
- Generalized: Covering a large proportion of the body, as in systemic drug reactions or viral exanthems.
- Localized: Restricted to a specific anatomical area, like contact dermatitis or a solitary insect bite.
- Acral: Affecting the extremities (hands, feet, ears, nose), seen in erythema multiforme or chilblains.
- Intertriginous: Occurring in skin folds (armpits, groin, under breasts), common in fungal infections or intertrigo.
- Flexural vs. Extensor: Predominance on flexor (bends of joints) or extensor (straightening side of joints) surfaces, as seen in atopic dermatitis (flexural) versus psoriasis (extensor).
- Symmetrical vs. Asymmetrical: Whether lesions appear on both sides of the body equally or preferentially on one side.
- Dermatomal: Following the distribution of a nerve root, characteristic of herpes zoster (shingles).
- Photosensitive: Occurring in sun-exposed areas, such as the malar rash of lupus or solar erythema.
Additional significant signs that can accompany erythema and are captured in various dermatological images include:
- Telangiectasias: Visible, small, dilated blood vessels, often seen in chronic sun damage or rosacea, contributing to background redness.
- Lichenification: Thickening of the skin with accentuation of skin markings, often due to chronic scratching, appearing as a consequence of persistent pruritic erythema.
- Atrophy: Thinning of the skin, which can occur as a result of chronic inflammation or prolonged use of potent corticosteroids on erythematous areas.
- Pigmentary changes: Post-inflammatory hyperpigmentation (darkening) or hypopigmentation (lightening) can follow resolution of erythematous lesions, especially in individuals with darker skin tones.
- Koebner phenomenon: The appearance of new lesions of a pre-existing dermatosis (e.g., psoriasis, lichen planus) at sites of skin trauma, which can manifest as linear erythema.
By meticulously observing and documenting these diverse signs, especially through visual aids like skin rash pictures, clinicians can effectively differentiate between the myriad causes of erythema and guide appropriate treatment strategies.
Early Erythema Photos
The early recognition of erythema symptoms is often critical for timely intervention and preventing disease progression. Early Erythema Photos are invaluable in illustrating the initial subtle changes that characterize the onset of various dermatological conditions. These initial presentations can be less pronounced than later stages, making careful observation paramount. Early erythema often appears as a faint pink or reddish discoloration, possibly accompanied by mild warmth or a subtle texture change, before evolving into more distinct patterns or lesions.
Understanding what to look for in the nascent stages of erythema can significantly impact diagnostic accuracy. Here’s how different conditions might present in their earliest phases:
- Early Erythema Migrans: In its very first hours or days, an erythema migrans lesion may simply be a small, non-descript red spot or papule at the site of a tick bite. It may be mistaken for a common insect bite reaction. The crucial differentiating factor, captured in serial early erythema pictures, is its slow, outward expansion, sometimes with subtle central clearing, over subsequent days.
- Early Erythema Multiforme (EM): Initial manifestations often involve small, symmetrical, fixed erythematous macules or papules, frequently on the extensor surfaces of the hands and feet, palms, and soles. These lesions might be mildly itchy or burning. The characteristic target morphology, if it develops, often evolves over 24-48 hours. Early detection focuses on these initial acral red spots.
- Early Contact Dermatitis: Upon initial exposure to an irritant or allergen, the skin may show very localized, faint pink to red discoloration, often accompanied by mild itching or a burning sensation. The borders might be indistinct. Over hours to days, this erythema becomes more pronounced, possibly developing vesicles, edema, and a sharper demarcation aligning with the contact area, as would be evident in progressive early skin rash images.
- Early Cellulitis: The initial signs of cellulitis can be subtle: a localized area of skin that feels slightly warm, tender, and appears as a faint blush or a patch of mild redness. The borders may be ill-defined. Without prompt treatment, this erythema rapidly intensifies in color and expands in size, accompanied by increased pain, warmth, and swelling, visible in evolving infection erythema photos.
- Early Solar Erythema (Sunburn): The skin initially shows a subtle pinkish tint and feels warm to the touch, often within a few hours of sun exposure. This early erythema can be easily overlooked, especially in individuals with darker skin tones where it might appear as a slight darkening or purplish hue. As damage progresses, the redness becomes more intense, painful, and may lead to blistering.
- Early Drug Eruptions: Many drug-induced erythematous rashes, such as morbilliform eruptions, begin as small, discrete, symmetrical, slightly raised red macules and papules, often appearing first on the trunk and then spreading peripherally. These initial lesions can resemble viral exanthems, making a detailed history of medication intake crucial.
- Early Viral Exanthems: Initial signs often involve diffuse, small, red macules or maculopapules, sometimes described as “blotchy.” These might first appear on the face or trunk and then spread, often associated with systemic symptoms like fever. The distribution and timing are key in differentiating these early viral rash photos.
- Early Urticaria (Hives): The earliest lesions of urticaria are small, individual, slightly raised, itchy red bumps or wheals that blanch with pressure. They can appear suddenly and are very transient, often disappearing within minutes to hours, only to be replaced by new lesions elsewhere.
- Early Rosacea: The first signs of rosacea typically involve transient facial flushing or redness, particularly across the nose, cheeks, forehead, and chin. This early erythema may be intermittent before becoming persistent. Over time, visible blood vessels (telangiectasias), papules, and pustules may develop, as observed in progressive facial erythema images.
- Early Folliculitis: This appears as small, individual, erythematous papules or pustules centered around hair follicles. The initial redness is often subtle, surrounding a tiny, irritated hair follicle, and can progress to more prominent inflamed lesions.
The ability to distinguish these subtle initial changes is essential for preventing the escalation of conditions, reducing discomfort, and initiating specific treatments where necessary. Public awareness campaigns and educational materials often utilize early erythema photos to help individuals and healthcare providers recognize these crucial initial signs.
Factors that can influence the appearance of early erythema include:
- Skin tone: Redness may be less obvious or appear as purplish/brownish discoloration on darker skin tones.
- Location: Some areas of the body may show redness more readily due to thinner skin or higher vascularity.
- Underlying cause: The speed and intensity of erythema onset depend heavily on the etiological agent (e.g., rapid onset for allergic reactions vs. slower for chronic inflammatory conditions).
- Individual inflammatory response: Genetic factors and overall health can influence how quickly and severely an individual develops an erythematous response.
Therefore, when reviewing dermatological images of early erythema, it’s vital to consider the context, patient history, and any associated symptoms to arrive at an accurate early diagnosis.
Skin rash Erythema Images
The term “skin rash” broadly encompasses any abnormal change in the skin’s texture or color, and erythema is a foundational component of many rashes. Skin rash Erythema Images vividly display the diverse appearances of red rashes, which can stem from myriad causes, including infections, allergic reactions, autoimmune diseases, and systemic illnesses. Analyzing these images requires attention to the detailed characteristics of the redness, associated lesions, distribution, and configuration.
Erythematous rashes are incredibly common and can range from benign, self-limiting conditions to serious, life-threatening diseases. Here, we categorize and describe various types of red rashes commonly depicted in erythematous skin images:
Maculopapular Erythematous Rashes:
- Morbilliform Rashes: These rashes consist of diffuse, confluent, or discrete erythematous macules and papules that resemble measles. They are a common presentation of viral exanthems (e.g., measles, rubella, parvovirus B19 – “slapped cheek” appearance, roseola infantum) and drug eruptions. The color is typically bright red to pink, often starting on the trunk or face and spreading.
- Scarlet Fever Rash: Characterized by diffuse erythema with tiny, sandpaper-like papules, giving the skin a rough texture. It often starts on the neck and chest and spreads, commonly associated with a “strawberry tongue.” This specific texture and generalized redness are key in scarlet fever erythema pictures.
- Pityriasis Rosea: Often starts with a “herald patch,” a solitary, oval, erythematous, slightly scaly plaque, usually on the trunk. Days to weeks later, smaller oval, pink-to-red macules and papules appear in a “Christmas tree” pattern on the trunk and proximal extremities, following the skin cleavage lines.
- Dengue Fever Rash: Can vary, but often includes a generalized erythematous rash, sometimes maculopapular, that may be preceded by facial flushing. Petechiae (small non-blanching red spots) or purpura may also be present, visible in tropical disease rash images.
Vesiculobullous Erythematous Rashes:
- Herpes Simplex (Cold Sores, Genital Herpes): Presents as clusters of erythematous vesicles on a red base, often painful and localized to specific areas (lips, genitals). The rapid progression from erythema to vesicles and then crusting is characteristic.
- Herpes Zoster (Shingles): Characterized by painful, erythematous papules and vesicles appearing in a dermatomal (nerve pathway) distribution, typically unilateral. The sharply demarcated red band of inflammation with clustered blisters is highly diagnostic in shingles rash images.
- Chickenpox (Varicella): Generalized erythematous rash with vesicles in different stages of development (“dewdrop on a rose petal”), starting on the trunk and spreading to the face and extremities. The widespread but varied lesions on an erythematous base are crucial visual cues.
- Bullous Pemphigoid: Large, tense bullae (blisters) on an erythematous or non-erythematous base, often intensely itchy, predominantly affecting the trunk and flexural areas. The intact, large blisters on red skin are striking in blistering rash images.
Pustular Erythematous Rashes:
- Acne Vulgaris: Characterized by erythematous papules, pustules, nodules, and cysts, primarily on the face, chest, and back. The inflammatory red lesions with central pus are common in acne images.
- Pustular Psoriasis: Can be localized or generalized, presenting as widespread sterile pustules on an erythematous base, often accompanied by fever and systemic symptoms. This severe form of psoriasis has distinct visual signs.
- Folliculitis: Erythematous papules and pustules centered around hair follicles, indicating inflammation or infection of the hair follicle.
Annular/Arcuate Erythematous Rashes:
- Tinea Corporis (Ringworm): An erythematous, annular (ring-shaped) plaque with an active, scaling, raised border and central clearing, caused by a dermatophyte fungal infection. The distinct ring shape with peripheral scaling is a key feature in fungal rash images.
- Granuloma Annulare: Smooth, firm, skin-colored, erythematous, or slightly violaceous papules coalescing into an annular configuration, often on the hands and feet. The lack of scaling differentiates it from tinea.
- Subacute Cutaneous Lupus Erythematosus (SCLE): Often presents as erythematous, annular, or polycyclic (multiple rings) plaques with mild scaling and central clearing, typically in sun-exposed areas.
Nodular Erythematous Rashes:
- Erythema Nodosum: As described earlier, tender, red to violaceous subcutaneous nodules, primarily on the shins.
- Deep Fungal Infections (e.g., sporotrichosis): Can present as erythematous, often ulcerative, nodules that may follow lymphatic channels.
Other Distinct Erythematous Rashes:
- Psoriasis Vulgaris: Characterized by well-demarcated, erythematous plaques covered with silvery scales, predominantly on extensor surfaces (elbows, knees, scalp, lower back). The redness combined with the thick scale is iconic in psoriasis pictures.
- Atopic Dermatitis (Eczema): In acute stages, presents as erythematous, edematous (swollen) patches and plaques with papules, vesicles, oozing, and crusting. In chronic stages, lichenification (skin thickening) and xerosis (dryness) dominate. The distribution in flexural areas (e.g., inner elbows, behind knees) is often key.
- Lupus Erythematosus (Cutaneous):
- Malar Rash (“Butterfly Rash”): Erythema across the bridge of the nose and malar eminences, sparing the nasolabial folds, a classic sign of systemic lupus erythematosus.
- Discoid Lupus Erythematosus: Chronic, well-demarcated, erythematous plaques with follicular plugging, adherent scaling, and atrophy, often leading to scarring and pigmentary changes, typically on the face, scalp, and ears.
- Seborrheic Dermatitis: Erythematous patches and plaques with greasy, yellowish scales, primarily in sebum-rich areas like the scalp, eyebrows, nasolabial folds, and chest. The combination of redness and greasy scale is visually distinctive.
- Erythrasma: A bacterial infection presenting as well-demarcated, reddish-brown patches with fine scaling, commonly in intertriginous areas like the groin or armpits. Fluoresces coral red under Wood’s lamp.
The vast spectrum of skin rash erythema images underscores the complexity of dermatological diagnosis, requiring a methodical approach to evaluating each visual cue. Detailed description of the rash, combined with patient history and other clinical findings, is essential for accurate identification and management of the underlying condition.
Erythema Treatment
The treatment of erythema is fundamentally dependent on identifying and addressing its underlying cause. Since erythema is a symptom, effective management requires an accurate diagnosis, often aided by careful examination of erythema symptoms pictures. Treatment strategies range from simple symptomatic relief to targeted therapies for specific conditions. The primary goals of erythema treatment are to reduce inflammation, alleviate associated symptoms (like pain or itching), prevent complications, and resolve the root cause.
Here’s a comprehensive overview of erythema treatment approaches, categorized by the etiology or general therapeutic modality:
1. Treatment for Infectious Causes of Erythema:
- Bacterial Infections:
- Antibiotics: For conditions like cellulitis, erysipelas, bacterial folliculitis, or Lyme disease (Erythema Migrans). Oral antibiotics (e.g., penicillin, cephalexin, doxycycline) are commonly used, with intravenous antibiotics reserved for severe cases.
- Topical Antibiotics: For localized superficial bacterial infections, such as mupirocin for impetigo.
- Viral Infections:
- Antivirals: For herpes simplex (acyclovir, valacyclovir) or herpes zoster (valacyclovir, famciclovir) to reduce severity and duration, especially if initiated early.
- Supportive Care: For most viral exanthems (e.g., measles, rubella, chickenpox), treatment is primarily symptomatic, including rest, hydration, and fever reducers (acetaminophen, ibuprofen).
- Fungal Infections:
- Antifungals: Topical agents (e.g., clotrimazole, miconazole) for localized superficial infections like tinea corporals. Oral antifungals (e.g., terbinafine, fluconazole) may be necessary for widespread or resistant cases.
- Parasitic Infections:
- Scabicides: For scabies, topical permethrin cream or oral ivermectin.
2. Treatment for Inflammatory and Immune-Mediated Causes:
- Topical Corticosteroids: These are the cornerstone for many inflammatory erythematous conditions, reducing redness, swelling, and itching.
- Indications: Eczema (atopic dermatitis, contact dermatitis), psoriasis, seborrheic dermatitis, lichen planus, mild forms of erythema annulare centrifugum.
- Potency: Available in varying strengths (low, medium, high, very high) and formulations (creams, ointments, lotions) chosen based on the severity of erythema, location, and patient age.
- Caution: Prolonged use, especially of potent steroids, can lead to side effects like skin thinning (atrophy), telangiectasias, striae, and secondary infections.
- Systemic Corticosteroids: Oral or injected corticosteroids (e.g., prednisone) are used for severe, widespread, or disabling inflammatory erythematous conditions.
- Indications: Severe acute contact dermatitis, severe erythema multiforme, widespread drug eruptions, severe flare-ups of psoriasis or eczema.
- Caution: Used for short durations due to significant potential side effects (e.g., weight gain, hypertension, diabetes, osteoporosis).
- Immunosuppressants/Immunomodulators: For chronic, severe inflammatory erythema not controlled by topical steroids.
- Indications: Severe psoriasis (methotrexate, cyclosporine), chronic eczema (tacrolimus, pimecrolimus, crisaborole – topical calcineurin inhibitors/PDE4 inhibitor), chronic urticaria (omalizumab – anti-IgE biologic).
- Biologic Therapies: Targeted treatments for specific pathways in immune-mediated diseases.
- Indications: Moderate to severe psoriasis (e.g., ustekinumab, secukinumab, ixekizumab), severe atopic dermatitis (dupilumab), chronic urticaria (omalizumab). These agents significantly reduce erythema and associated symptoms.
- NSAIDs (Nonsteroidal Anti-inflammatory Drugs): Oral NSAIDs (e.g., ibuprofen, naproxen) can help reduce pain and inflammation associated with some erythematous conditions.
- Indications: Erythema nodosum, sunburn, some forms of vasculitis.
- Antihistamines: Reduce itching and can help with allergic reactions.
- Indications: Urticaria, insect bites, allergic contact dermatitis, atopic dermatitis (especially sedating antihistamines at night for sleep).
- Retinoids:
- Topical Retinoids (e.g., tretinoin, adapalene): For acne vulgaris and sometimes for photodamage, reducing inflammation and promoting cell turnover.
- Oral Retinoids (e.g., isotretinoin, acitretin): For severe acne, severe psoriasis, and some forms of cutaneous lupus. Highly effective but with significant side effect profiles.
- Rosacea-Specific Treatments:
- Topical Agents: Metronidazole, azelaic acid, brimonidine (for persistent facial redness).
- Oral Agents: Low-dose doxycycline (anti-inflammatory effects), isotretinoin for severe papulopustular rosacea.
- Laser/Light Therapy: Pulsed dye laser (PDL) for telangiectasias and persistent erythema.
3. Treatment for Physical Causes of Erythema:
- Sunburn (Solar Erythema):
- Cool Compresses: To soothe the skin and reduce heat.
- Moisturizers: Emollients to hydrate the skin and prevent peeling.
- NSAIDs: For pain and inflammation.
- Topical Corticosteroids: Mild-to-moderate strength for short periods to reduce inflammation.
- Prevention: Sun protection (sunscreen, protective clothing, shade) is paramount.
- Erythema Ab Igne:
- Removal of Heat Source: Essential to prevent further damage and allow the erythema to fade.
- Emollients: To soothe the skin.
- Topical Retinoids: May help improve residual pigmentation or skin texture.
- Erythema Pernio (Chilblains):
- Re-warming: Gradual re-warming of affected areas.
- Avoidance of Cold: Protection from further cold exposure (warm clothing, gloves, socks).
- Topical Corticosteroids: For symptomatic relief of itching and inflammation.
- Vasodilators: Oral nifedipine may be prescribed for severe or recurrent cases.
4. General Supportive Care and Lifestyle Modifications:
- Emollients and Moisturizers: Essential for maintaining skin barrier function, especially in conditions with dry, inflamed skin like eczema or psoriasis.
- Cool Compresses/Baths: Provide symptomatic relief for itching and burning associated with various erythematous rashes.
- Avoidance of Triggers: Identifying and avoiding known irritants (in contact dermatitis), allergens, specific foods, or environmental factors (e.g., heat, cold, stress for rosacea).
- Skin Protection: Wearing loose, breathable clothing; avoiding harsh soaps or detergents; and protecting affected areas from trauma.
- Rest and Elevation: For lower limb erythema (e.g., cellulitis, erythema nodosum) to reduce swelling.
The selection of erythema treatment is a nuanced process that takes into account the specific diagnosis, severity, extent of the erythema, patient age, comorbidities, and potential side effects of medications. Often, a combination of therapies is employed to achieve optimal outcomes. Regular follow-up with a healthcare provider, especially when examining changes in Erythema symptoms pictures over time, is crucial to monitor treatment effectiveness and adjust the plan as needed.