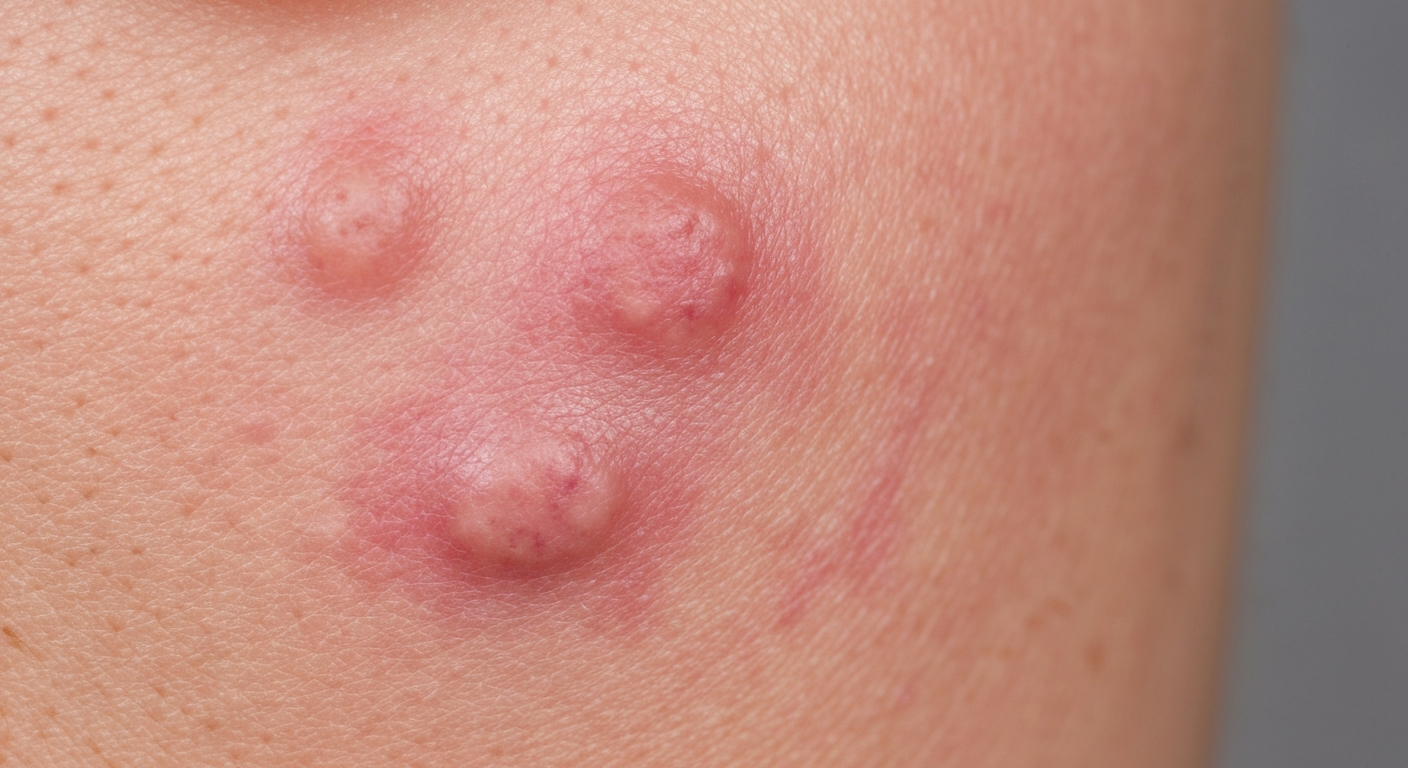
For those seeking to understand What Does Genital Herpes Look Like Symptoms Pictures, this guide provides a direct and comprehensive visual description of the condition’s manifestations. We delve into the specific appearance of sores, blisters, and rashes associated with genital herpes outbreaks, providing crucial details on progression and common locations.
Genital herpes Symptoms Pictures
Genital herpes symptoms often present as a cluster of small, painful blisters that eventually break open to form shallow ulcers. Understanding the visual progression is key for identifying potential genital herpes. Initially, the affected skin area may feel itchy, tingly, or burning before any visible lesions appear. This prodromal stage of genital herpes is crucial for early recognition. Within hours to days, small red bumps or papules emerge. These are the earliest visible signs of a primary genital herpes outbreak or a recurrent episode.
These red bumps rapidly evolve into tiny, fluid-filled vesicles, which are characteristic genital herpes blisters. The fluid inside these blisters is typically clear or yellowish. They are often grouped together in a tight cluster, resembling a small bunch of grapes. The size of these blisters can vary, but they are generally small, often 1-3 millimeters in diameter. The skin around these blisters is usually red, swollen, and very tender to the touch. The specific appearance can differ based on the location, skin type, and immune response of the individual. For instance, on moist mucosal surfaces like the labia or penis, the blisters might rupture more quickly due to friction and moisture.
As the genital herpes infection progresses, these delicate blisters rupture. This typically happens within a few days of their formation. The rupture of the vesicles creates open sores or genital herpes ulcers. These ulcers are usually shallow, round or oval, and have a reddish base. They can be quite painful, especially when exposed to urine, friction from clothing, or during sexual activity. The edges of the ulcers may appear somewhat irregular or well-defined. Multiple ulcers may coalesce, forming larger, more irregular ulcerated areas. This phase is often the most symptomatic and visually distinct aspect of a genital herpes outbreak.
Following the ulceration phase, the sores begin to dry out and scab over. The scabs are typically yellowish or brownish and form a protective crust over the healing skin. This genital herpes healing process indicates that the viral shedding is decreasing, and the skin is starting to repair itself. The scabs will eventually fall off, revealing new, healthy skin underneath. In some cases, temporary discoloration (post-inflammatory hyperpigmentation or hypopigmentation) may remain in the affected area, but scarring is rare unless there was significant secondary bacterial infection or trauma.
Specific visual characteristics associated with genital herpes outbreaks include:
- Clustering: Lesions typically appear in a localized group rather than spread out individually.
- Erythema: Redness and inflammation surrounding the active lesions.
- Tenderness: The affected area is usually very sensitive and painful.
- Progression: The characteristic sequence of red bumps -> fluid-filled blisters -> painful ulcers -> crusting scabs -> healing.
- Location Variation: Appearance can subtly change depending on whether the lesions are on keratinized skin (e.g., shaft of the penis, outer labia) versus mucosal surfaces (e.g., glans, inner labia, vaginal wall, anus). On mucosal surfaces, blisters might be less prominent and rupture faster, leading directly to ulcers.
- Recurrence Patterns: Subsequent outbreaks often present similarly to the primary infection but may be milder, shorter in duration, and involve fewer lesions.
- Atypical Presentations: Sometimes, especially in individuals with compromised immune systems or in less common locations, genital herpes can present atypically, such as fissures, persistent redness, or even just itching without overt blistering.
Signs of Genital herpes Pictures
Recognizing the signs of genital herpes is critical for accurate diagnosis and management. The initial signs of a genital herpes outbreak, whether it’s the first episode or a recurrence, are often subtle before progressing to more overt lesions. Patients might first notice a tingling, itching, or burning sensation in the genital or anal area. This sensation, known as a prodrome, serves as an early warning sign that an outbreak is imminent. This early symptom of genital herpes typically precedes the visible skin changes by hours or a day.
Once visible signs emerge, they commonly begin as small, red bumps or papules. These bumps are localized to the area where the virus is active. Within a short period, often less than 24 hours, these red bumps transform into classic genital herpes vesicles. These vesicles are small, fluid-filled sacs that are typically clear or yellowish. They tend to be clustered together, giving them a distinctive appearance often described as a “cluster of pearls” or “dewdrops on a rose petal” due to their glistening, fluid-filled nature and surrounding redness.
The locations where these signs appear are highly indicative of genital herpes. For women, lesions commonly appear on the labia majora and minora, vaginal entrance, perineum, buttocks, and sometimes on the cervix or inside the vagina. For men, common sites include the shaft of the penis, glans, scrotum, inner thighs, and buttocks. Lesions can also appear around the anus in both sexes, particularly in individuals engaging in anal intercourse. The exact genital herpes lesion location helps narrow down the diagnosis.
As the vesicles burst, they leave behind shallow, raw, and often very painful sores or ulcers. These genital herpes sores are characterized by their reddish base and can be quite tender. The raw surface is susceptible to secondary infection, although this is not a direct sign of herpes itself. The number of ulcers can vary significantly; a primary outbreak might involve numerous widespread ulcers, whereas recurrent outbreaks typically involve fewer, more localized lesions. The ulcers weep clear fluid before starting to dry and form crusts.
Beyond the visible lesions, other systemic signs can accompany an initial genital herpes outbreak, particularly a severe primary episode. These include flu-like symptoms such as fever, headache, muscle aches (myalgia), and swollen and tender lymph nodes in the groin area (inguinal lymphadenopathy). These systemic signs are less common in recurrent outbreaks but can still occur. The presence of these systemic symptoms alongside the characteristic genital lesions strongly points towards a primary genital herpes infection.
Key visual indicators to look for:
- Clustered Vesicles: Small, clear or yellowish fluid-filled blisters grouped closely together.
- Erosions/Ulcers: Shallow, painful open sores with a reddish base formed after blisters rupture.
- Perilesional Erythema: Redness and inflammation around the lesions.
- Edema: Swelling of the affected genital tissues.
- Crusting: Yellowish or brownish scabs forming over healing ulcers.
- Genital vs. Perianal: Distribution in the genital region, perineum, inner thighs, or buttocks.
- Mucosal Involvement: Lesions on moist tissues (vagina, glans, anus) may appear less blister-like and more as erosions directly.
- Absence of Pustules: True herpes lesions are vesicular (fluid-filled), not typically pustular (pus-filled), unless secondarily infected.
- Symmetry/Asymmetry: Outbreaks can be unilateral or bilateral, though often localized to one side or a specific patch.
Early Genital herpes Photos
The early stages of genital herpes are crucial for identification, as symptoms progress rapidly. What might appear as a minor irritation can quickly evolve into a full-blown outbreak. The very first early genital herpes photos would often capture the prodromal stage, though these are typically not visible skin changes. Instead, they refer to subjective sensations like itching, tingling, or burning in the genital or anal region. This heralds the impending eruption of lesions and is a critical period for initiating antiviral therapy to potentially abort or significantly lessen an outbreak.
Once visible signs appear, the earliest manifestations are typically small, reddish bumps, medically termed papules. These first signs of genital herpes are often mistaken for insect bites, razor bumps, or other minor skin irritations. They can be singular, but more commonly, they appear as a small cluster of closely spaced red bumps. These initial red spots usually do not contain fluid yet. They are simply areas of inflammation and early viral replication beneath the skin surface. The skin around these red bumps may feel warm or look slightly swollen.
Within hours to a day, these red bumps transform into the hallmark early genital herpes blisters. These are small, clear or yellowish fluid-filled vesicles. They are typically very fragile and can be quite numerous in the affected area, often appearing in groups or clusters. The fluid within the vesicles is rich in viral particles, making this stage highly contagious. The size of these early blisters is usually quite small, often only 1-2 millimeters in diameter, and they are surrounded by a distinct red halo, indicating local inflammation.
Locations for these early lesions are consistent with typical genital herpes sites. For women, the early symptoms of herpes on vulva, inner thighs, or around the anus are common. For men, the shaft of the penis, glans, or scrotum are frequent sites for the initial appearance of these clustered red bumps and vesicles. It’s important to differentiate these from other conditions that might cause similar-looking bumps, such as folliculitis or contact dermatitis, which usually lack the clustering and rapid progression to fluid-filled vesicles seen in herpes.
The pain and discomfort associated with these early lesions can be significant. Even before the blisters fully rupture, the nerve endings in the affected area are highly sensitized. Walking, sitting, urinating (if lesions are near the urethra), or having any friction from clothing can intensify the discomfort. Swollen lymph nodes in the groin may also begin to develop during this very early stage, indicating the body’s immune response to the viral infection. Genital herpes primary outbreak photos often depict more widespread and severe early lesions compared to recurrent episodes, which tend to be more localized and milder.
Detailed breakdown of early visual signs:
- Prodromal Sensations: Itching, tingling, burning, or pain in the area before any visible lesions. This is the earliest warning.
- Red Papules: Small, localized red bumps that appear on the skin or mucosal surface. Often clustered.
- Vesicle Formation: Rapid development of these papules into small, clear or yellowish fluid-filled blisters (vesicles).
- Clustering Pattern: The distinct grouping of multiple vesicles together, often resembling a small bunch of grapes.
- Erythematous Base: Redness and inflammation surrounding each individual blister and the cluster as a whole.
- Edema: Mild to moderate swelling of the surrounding tissue, contributing to discomfort.
- Tenderness: The area becomes highly sensitive and painful to touch.
- Location Specificity: Appearing on genitals, perineum, inner thighs, or buttocks.
- Flu-like Symptoms: In a primary infection, fever, body aches, and headache may accompany the early skin lesions.
- Lymphadenopathy: Swollen and tender lymph nodes in the groin, indicating an active immune response.
Skin rash Genital herpes Images
When discussing a “skin rash” in the context of genital herpes, it’s important to understand that herpes does not typically present as a widespread, diffuse rash like measles or eczema. Instead, the genital herpes rash refers to the characteristic localized outbreak of clustered blisters and subsequent ulcers. These lesions form a distinct pattern that is visually different from many other common skin conditions, making photographic identification crucial for understanding its appearance.
A typical herpes skin rash begins as small red bumps, which quickly develop into fluid-filled vesicles. These vesicles are the most visually diagnostic feature of an active herpes outbreak. They are usually clear or yellowish, tense, and grouped tightly together on an inflamed, reddened base. The size of each vesicle is generally small, ranging from 1 to 3 millimeters. This clustering pattern is a key differentiator from conditions like molluscum contagiosum (which often presents as scattered, flesh-colored papules with a central dimple) or genital warts (which are typically flesh-colored, cauliflower-like growths).
As the vesicles rupture, they give way to shallow, painful erosions or ulcers. These genital herpes ulcers pictures show raw, reddish areas that weep fluid before forming a crust. The margins of these ulcers can be somewhat irregular. The entire “rash” area, encompassing the cluster of lesions, is typically acutely painful, tender, and often accompanied by swelling (edema) of the surrounding genital tissues. The inflammation contributes significantly to the visual redness and discomfort observed in genital herpes pictures.
The progression of this localized “rash” is rapid: from red bumps to vesicles, then to ulcers, and finally to crusts and healing. This predictable evolution over 7-14 days (for recurrent outbreaks) or 2-4 weeks (for primary outbreaks) is characteristic. The resolution often leaves no scar, though temporary changes in skin pigmentation (lighter or darker spots) may persist for a while. The genital herpes rash on vulva or penis often appears on areas prone to friction or nerve endings where the virus resides. For instance, lesions on the labia or glans penis may appear particularly raw due to moisture and movement.
Differentiation from other rashes is vital. For example, a fungal infection (candidiasis) typically presents as a red, itchy rash with satellite lesions that are not vesicular. Allergic contact dermatitis might show redness and intense itching but usually without the characteristic clustered vesicles and ulcers. Syphilitic chancres, while also ulcerative, are typically solitary, painless, and have firm, raised borders, unlike the painful, clustered, shallow ulcers of herpes.
Key descriptive points for the genital herpes skin rash:
- Clustered Vesicles: The defining feature is a group of small, fluid-filled blisters on a reddened base. These are not scattered.
- Erythematous Edema: Significant redness and swelling around the affected patch of skin.
- Rapid Progression: Quick transition from red bumps to blisters, then to open sores.
- Ulcer Characteristics: Shallow, round/oval, reddish base, often painful.
- Crusting Phase: Formation of yellowish-brown scabs over healing sores.
- Localized Nature: The rash is typically confined to a specific, relatively small area (e.g., a patch on the labia, penis, or buttocks), rather than being widespread.
- Painful: Unlike many rashes that are primarily itchy, herpes lesions are notably painful.
- Absence of Pus: Unless secondarily infected, the fluid in herpes blisters is clear, not purulent.
- Associated Symptoms: Local tingling, burning, or itching often precedes the visible rash.
- Mucosal Appearance: On mucous membranes (e.g., inside the mouth, vagina, anus), the blisters might be more transient, quickly eroding into ulcers due to the delicate nature of the tissue.
Genital herpes Treatment
While this article primarily focuses on What Does Genital Herpes Look Like Symptoms Pictures, understanding the treatment options for genital herpes is crucial, as they directly impact the appearance and duration of outbreaks. Antiviral medications are the cornerstone of genital herpes treatment. These medications work by inhibiting the replication of the herpes simplex virus (HSV), thereby reducing the severity, duration, and frequency of outbreaks. It’s important to note that antivirals do not cure genital herpes; the virus remains dormant in nerve cells. However, they significantly alter the visual manifestation and impact of the disease.
The primary antiviral medications used for genital herpes include acyclovir, valacyclovir, and famciclovir. These drugs can be prescribed in two main ways: episodic therapy or suppressive therapy.
Episodic Therapy for Genital Herpes:
Episodic therapy involves taking antiviral medication only when an outbreak occurs or is imminent. The goal is to shorten the duration of the outbreak and reduce the severity of symptoms. For this to be effective, treatment should ideally begin during the prodromal stage (when tingling, itching, or burning sensations are felt) or at the very first sign of lesion appearance (red bumps). If started early:
- Reduced Lesion Progression: The antiviral medication can sometimes abort the outbreak, meaning the red bumps may not fully develop into fluid-filled blisters, or the blisters may be fewer and smaller.
- Faster Healing: If blisters and ulcers do form, they tend to heal more quickly, often by several days, compared to untreated outbreaks. This means the stages of blistering, ulceration, and crusting are accelerated.
- Less Severe Appearance: The number of lesions is usually reduced, and the overall inflammation (redness and swelling) is diminished.
- Decreased Pain: The pain associated with the lesions is often less intense and resolves faster.
- Reduced Viral Shedding: The period during which the virus is present on the skin surface (and thus contagious) is shortened, though abstinence is still recommended during active outbreaks.
Suppressive Therapy for Genital Herpes:
Suppressive therapy involves taking a daily dose of antiviral medication to prevent outbreaks. This approach is typically recommended for individuals who experience frequent or severe recurrent outbreaks (e.g., six or more outbreaks per year) or those who wish to reduce the risk of transmitting the virus to a partner. The impact on the visual appearance of genital herpes is profound:
- Fewer Outbreaks: The primary benefit is a significant reduction (by 70-80% or more) in the frequency of visible outbreaks. Many individuals on suppressive therapy experience no outbreaks at all for extended periods.
- Milder Outbreaks: If an outbreak does occur while on suppressive therapy, it is usually much milder in appearance. Lesions may be fewer, smaller, and resolve more quickly than typical recurrent outbreaks.
- Reduced Prodrome: The prodromal symptoms (tingling, itching) that precede visible lesions may also be less frequent or less intense.
- Reduced Asymptomatic Shedding: Suppressive therapy also reduces asymptomatic viral shedding, meaning the virus is present on the skin without visible lesions less often, thereby reducing the risk of transmission, although it does not eliminate it entirely.
Non-Pharmacological Approaches and Symptomatic Relief:
While antivirals are key, symptomatic relief can also improve the comfort and appearance during an outbreak:
- Pain Management: Over-the-counter pain relievers such as ibuprofen or acetaminophen can reduce the discomfort associated with genital herpes lesions. Topical anesthetics (e.g., lidocaine cream) can also be applied directly to the sores to numb the area, making the patient more comfortable.
- Hygiene: Keeping the affected area clean and dry is important. Gentle washing with plain water and mild soap can prevent secondary bacterial infections, which could alter the visual appearance of the lesions (e.g., introduce pus or further inflammation). Patting the area dry instead of rubbing is recommended.
- Loose Clothing: Wearing loose-fitting cotton underwear and clothing can reduce friction and irritation on the lesions, promoting faster healing and preventing further pain or rupture of blisters.
- Sitz Baths: Soaking in warm water (sitz bath) can soothe painful sores, particularly in the perianal and perineal regions. Adding Epsom salts to the bath may also provide some relief and help dry out lesions.
- Avoid Irritants: Avoiding scented soaps, douches, and harsh cleansers on the genital area during an outbreak is crucial, as these can further irritate the sensitive skin and delay healing.
The goal of genital herpes treatment is not just to manage the symptoms but to improve the overall quality of life by reducing the physical and psychological impact of outbreaks. By effectively treating genital herpes, individuals can significantly control the frequency, severity, and visible signs of the condition, leading to less discomfort and a reduced risk of transmission.