Many individuals search for What Does A Goiter Look Like Symptoms Pictures to understand this common thyroid condition. Recognizing the visual signs and associated discomfort is crucial for early detection and management, offering insights into potential underlying thyroid dysfunction.
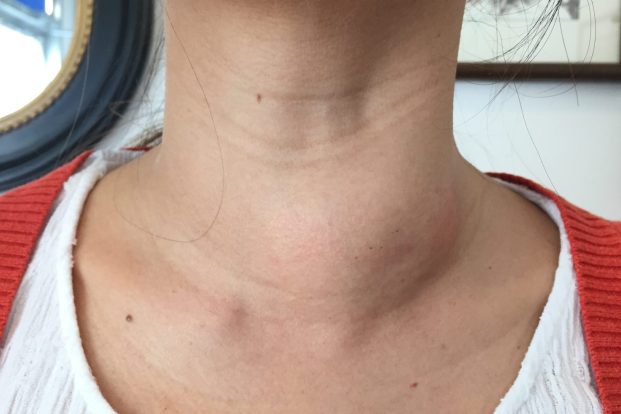
Goiter Symptoms Pictures
Understanding the visual manifestations of a goiter is paramount for early recognition. A goiter refers to an abnormal enlargement of the thyroid gland, which is located at the base of your neck. The appearance can vary significantly, from a barely perceptible swelling to a massive, disfiguring mass. When looking at goiter symptoms pictures, individuals should observe the anterior neck region for any asymmetry or protrusion. Diffuse goiters present as a generalized, smooth enlargement of the entire thyroid gland, often giving the neck a full or thick appearance. This uniform swelling can be particularly noticeable when the head is tilted back, making the goiter more prominent.
Nodular goiters, on the other hand, are characterized by one or more distinct lumps or nodules within the thyroid gland. These nodules can be clearly palpable and sometimes visible, appearing as localized bumps on one or both sides of the Adam’s apple area. A single thyroid nodule might create an asymmetrical bulge, whereas a multinodular goiter, featuring multiple nodules, often results in a more irregular and lumpy neck contour. In advanced cases, particularly with large multinodular goiters, the neck may appear grossly distorted, sometimes extending down into the chest cavity (substernal goiter) or pushing the trachea aside.
Beyond the primary visual symptom of neck swelling, goiter symptoms pictures often illustrate the secondary effects of this enlargement. A significant goiter can exert pressure on surrounding structures in the neck, leading to a range of uncomfortable symptoms. These include:
- Difficulty Swallowing (Dysphagia): As the goiter presses against the esophagus, individuals may experience a sensation of food getting stuck in their throat or difficulty in swallowing solid foods. This can range from mild discomfort to severe impediment, visible in how a person might strain or cough during meals.
- Difficulty Breathing (Dyspnea): Pressure on the trachea (windpipe) can cause shortness of breath, especially when lying down or during physical exertion. This may manifest as wheezing, a whistling sound during breathing, or a feeling of constriction in the throat.
- Hoarseness or Voice Changes (Dysphonia): If the goiter compresses the recurrent laryngeal nerve, which controls vocal cord movement, it can lead to a change in voice quality, often becoming hoarse, raspy, or breathy. In severe cases, partial or complete vocal cord paralysis can occur.
- Coughing: A chronic cough or a persistent tickle in the throat, not associated with a cold, can be a sign of tracheal irritation due to the enlarged thyroid.
- Neck Tightness or Discomfort: A general feeling of fullness, pressure, or tightness in the neck is a common complaint. This discomfort can range from a dull ache to a more significant pain, especially if there’s bleeding into a cyst or rapid enlargement of a nodule.
- Venous Congestion: In very large goiters, particularly substernal ones, compression of the neck veins can lead to swelling of the face, engorgement of neck veins, and sometimes a bluish discoloration (cyanosis) of the facial skin, especially when raising the arms (Pemberton’s sign).
These visual and symptomatic indicators are crucial when evaluating goiter symptoms pictures for potential thyroid enlargement. The overall appearance of the neck, coupled with patient-reported symptoms, provides vital clues for medical professionals.
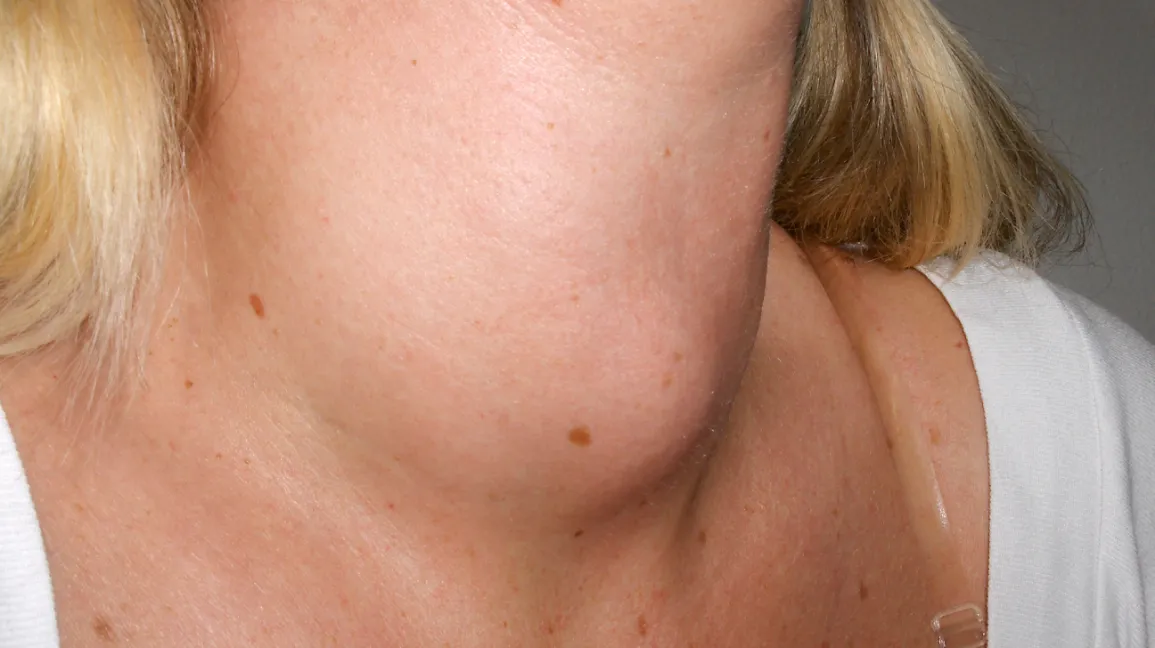
Signs of Goiter Pictures
When examining signs of goiter pictures, it’s important to differentiate between the goiter itself and the broader systemic signs of underlying thyroid dysfunction. While a visibly enlarged thyroid is the most direct sign, a goiter is often a manifestation of either hyperthyroidism (overactive thyroid) or hypothyroidism (underactive thyroid), each with its distinct set of accompanying physical signs. These broader signs can also be captured in signs of goiter pictures, reflecting the systemic impact of thyroid hormone imbalance.
For individuals with a hyperthyroid goiter, commonly seen in conditions like Graves’ disease, the accompanying signs can be profound and widely distributed across the body. These signs, often captured in illustrative medical imagery, include:
- Exophthalmos (Bulging Eyes): A classic sign of Graves’ ophthalmopathy, where the eyes appear to protrude from their sockets. This can be asymmetrical and is often accompanied by gritty sensation, light sensitivity, double vision, and redness of the eyes. The eyelids may also retract, giving a wide-eyed or staring appearance.
- Tremors: Fine tremors, particularly noticeable in the hands, can be observed. This involuntary shaking is more pronounced when extending the fingers and is a hallmark of an overactive metabolism.
- Weight Loss Despite Increased Appetite: A paradoxical weight loss despite eating more is a common sign of hyperthyroidism, as the body’s metabolic rate is significantly elevated.
- Heat Intolerance and Increased Sweating: Individuals may appear flushed and sweat excessively, even in cool environments, due to their heightened metabolic activity.
- Rapid Heart Rate (Tachycardia) or Palpitations: An elevated heart rate at rest or a feeling of the heart racing or pounding is a significant cardiovascular sign.
- Muscle Weakness: Proximal muscle weakness, affecting the thighs and upper arms, can be observed, making it difficult to climb stairs or lift objects.
- Anxiety, Irritability, and Restlessness: Behavioral changes are common, reflecting the overstimulation of the nervous system.
- Warm, Moist Skin: The skin often feels unusually warm and damp to the touch, another indicator of increased metabolic heat production.
- Hair Changes: Hair may become fine, brittle, and prone to excessive shedding or thinning.
- Onycholysis (Plummer’s Nails): Separation of the nail from the nail bed, particularly noticeable on the ring fingers, can be seen in some cases.
Conversely, signs of goiter pictures in the context of hypothyroidism, often associated with Hashimoto’s thyroiditis, present a different spectrum of systemic effects:
- Puffy Face (Myxedema): A characteristic puffiness, especially around the eyes and in the face, due to fluid retention and accumulation of hyaluronic acid in the skin and subcutaneous tissues. The eyelids may also appear swollen.
- Weight Gain: Unexplained weight gain, despite normal or reduced food intake, is a common sign of a slowed metabolism.
- Cold Intolerance: Individuals often complain of feeling cold, even in warm environments, due to decreased heat production.
- Fatigue and Sluggishness: Persistent tiredness, low energy levels, and a general feeling of being slowed down are prevalent.
- Bradycardia (Slow Heart Rate): The heart rate may be noticeably slower than normal.
- Dry, Coarse Skin and Hair: The skin often appears dry, scaly, and cool to the touch. Hair can become coarse, brittle, and prone to thinning, including loss of the outer third of the eyebrows (Madarosis).
- Constipation: A common gastrointestinal symptom due to slowed digestive processes.
- Depression and Impaired Memory: Cognitive and mood disturbances are frequently observed, impacting daily functioning.
- Deepening Voice: Swelling of the vocal cords can lead to a lower-pitched, hoarse voice.
These detailed systemic signs, when observed in conjunction with an enlarged thyroid, significantly aid in diagnosing the underlying thyroid disorder. Therefore, a comprehensive evaluation of signs of goiter pictures must extend beyond just the neck and consider these broader physiological manifestations.
Early Goiter Photos
Examining early goiter photos can be challenging because the initial stages of thyroid enlargement are often subtle and might not be immediately obvious to the untrained eye. Unlike late-stage goiters that present as dramatic neck swellings, early goiter photos typically show minimal changes in neck contour. The thyroid gland is naturally located in a somewhat hidden position at the base of the neck, overlying the trachea, making small enlargements difficult to spot without careful inspection or palpation.
In many early goiter photos, the most common visual cue might be a slight fullness or thickening in the lower anterior neck, just above the collarbones. This might be more apparent when the person swallows, as the enlarged gland moves up and down. Sometimes, the swelling is only visible when the neck is extended or when viewed from a specific angle, such as in profile. The skin over the thyroid area usually remains normal in appearance, without redness or tenderness, unless there is an inflammatory process or rapid hemorrhage into a nodule.
Early goiter symptoms often precede any clearly visible swelling. Patients might report a sensation of a “lump in the throat” (globus sensation), even if nothing is outwardly visible. This feeling can be particularly bothersome when swallowing or when wearing tight collars or necklaces. Other early, non-specific symptoms that might prompt a closer look, potentially leading to the discovery of an early goiter, include:
- Mild Dysphagia: A subtle difficulty or discomfort when swallowing, especially large pills or dry foods. This is due to slight pressure on the esophagus, not yet severe enough to cause overt blockage.
- Persistent Throat Clearing: An unconscious attempt to relieve a feeling of irritation or foreign body sensation in the throat.
- Subtle Voice Changes: A slight alteration in voice quality, such as mild hoarseness or a tendency for the voice to tire quickly, which might not be pronounced enough to be immediately recognized as a medical issue.
- Mild Neck Discomfort: A vague sensation of pressure or tightness in the neck, particularly after prolonged speaking or specific head movements.
- Palpable Nodule: Often, an early goiter is detected not visually but through palpation during a routine physical examination, where a doctor feels a small nodule or a diffuse enlargement that hasn’t yet become visible.
For individuals residing in iodine-deficient areas, early goiter photos might show a more generalized, diffuse enlargement, even if subtle. This is because iodine deficiency often leads to a compensatory hyperplasia (increase in cell number) of the thyroid gland in an attempt to capture more iodine for hormone production. In autoimmune conditions like Hashimoto’s thyroiditis, the early goiter can also be diffuse but might feel more firm or rubbery upon palpation. Graves’ disease, on the other hand, frequently presents with a diffuse, often softer goiter, sometimes accompanied by a palpable thrill or audible bruit over the gland due to increased blood flow.
The progression from early goiter to a more prominent one is variable. Factors influencing this progression include the underlying cause (e.g., persistent iodine deficiency, growth of a benign nodule, autoimmune activity), patient age, and hormonal influences. Therefore, vigilance for even these subtle changes and non-specific symptoms is key for identifying an early goiter. Medical imaging techniques such as ultrasound are often the definitive tools for detecting and characterizing early goiters that are not readily apparent in early goiter photos.
Skin rash Goiter Images
While a goiter itself is an enlargement of the thyroid gland, the underlying thyroid dysfunction can manifest in various dermatological conditions. Therefore, when discussing “skin rash goiter images,” we are primarily referring to skin manifestations associated with hyperthyroidism or hypothyroidism that often accompany a goiter. These skin changes can be significant diagnostic clues and are important to recognize.
Skin Manifestations in Hyperthyroidism (often with Goiter):
Conditions like Graves’ disease, a common cause of hyperthyroidism and goiter, are frequently associated with specific skin changes:
- Pretibial Myxedema (Thyroid Dermopathy): This is the most specific skin manifestation of Graves’ disease. In pretibial myxedema images, one would typically see thickened, waxy-appearing skin, often with a reddish-brown or yellowish discoloration, most commonly on the shins (pretibial area). The texture can be described as “peau d’orange” (orange peel) or “cobblestone” in appearance. It is caused by the accumulation of hyaluronic acid and chondroitin sulfate in the dermis and subcutaneous tissue. While most common on the shins, it can rarely affect other areas like the feet, hands, face, or trunk. The affected skin is typically non-pitting, meaning it doesn’t leave an indentation when pressed.
- Thyroid Acropachy: A rare but severe manifestation of Graves’ disease, often occurring in conjunction with pretibial myxedema and ophthalmopathy. Thyroid acropachy images show clubbing of the fingers and toes (bulbous enlargement of the fingertips), swelling of the digits, and periosteal new bone formation (abnormal bone growth) in the hands and feet. The nails may also appear curved.
- Warm, Moist, Velvety Skin: Due to increased blood flow and metabolic rate, the skin of hyperthyroid individuals often feels unusually warm, smooth, and moist to the touch. This can be generalized across the body.
- Palmar Erythema: Redness of the palms of the hands, a common finding in hyperthyroidism, caused by increased peripheral vasodilation.
- Diffuse Hair Loss (Telogen Effluvium): Hair may become fine, soft, and prone to diffuse shedding, often leading to a general thinning of the scalp hair. The hair texture can also change, becoming more brittle.
- Onycholysis (Plummer’s Nails): Separation of the nail plate from the nail bed, usually at the distal free edge, commonly affecting the fourth and fifth digits. The nails may also appear thin and brittle.
- Pruritus (Itching): Generalized itching without a specific rash can occur, possibly due to increased mast cell degranulation.
- Hyperpigmentation: Rarely, diffuse skin darkening can occur, mimicking Addison’s disease, but this is less common than in hypothyroidism.
- Urticaria and Angioedema: Chronic hives (urticaria) and deeper swelling (angioedema) have been associated with hyperthyroidism, possibly due to autoimmune mechanisms.
- Vitiligo: An autoimmune condition characterized by depigmented patches of skin. While not directly caused by hyperthyroidism, it is frequently associated with other autoimmune diseases, including Graves’ disease and Hashimoto’s thyroiditis, so images of vitiligo may be seen alongside a goiter.
Skin Manifestations in Hypothyroidism (often with Goiter):
Hypothyroidism, often caused by Hashimoto’s thyroiditis which can also present with a goiter, leads to a different set of skin changes:
- Dry, Coarse, and Cold Skin: The skin becomes noticeably dry, rough, and scaly due to decreased sebaceous gland activity and reduced sweating. It also feels cool to the touch because of decreased blood flow and metabolic rate.
- Generalized Myxedema: Similar to pretibial myxedema but generalized, this refers to the accumulation of mucopolysaccharides in the dermis, leading to non-pitting puffiness, especially noticeable in the face (puffy eyelids, thickened lips, broad nose). The hands and feet can also appear swollen and doughy. This is a classic feature in images of severe hypothyroidism.
- Yellowish Skin Discoloration (Carotenemia): Impaired conversion of beta-carotene to vitamin A leads to accumulation of carotene in the stratum corneum, giving the skin a yellow-orange tint, particularly noticeable on the palms, soles, and nasolabial folds.
- Brittle Nails: Nails become fragile, slow-growing, and may show longitudinal ridges.
- Hair Loss: Diffuse hair thinning, often with coarse, dry, and brittle hair. A classic sign is the loss of the outer third of the eyebrows (Madarosis). Scalp hair may also become sparse.
- Pallor: The skin may appear pale due to anemia (common in hypothyroidism) and vasoconstriction.
- Delayed Wound Healing: Slower cell turnover and impaired immune function can lead to delayed healing of skin injuries.
- Pruritus: Less common than in hyperthyroidism, but dry skin can lead to itching.
- Ichthyosis-like changes: Severe dryness and scaling can mimic ichthyosis, a group of genetic skin disorders characterized by very dry, scaly skin.
When reviewing skin rash goiter images, it is essential to consider the entire clinical picture and underlying thyroid function tests to establish a definitive diagnosis. These dermatological manifestations are crucial complementary signs for diagnosing thyroid disorders.
Goiter Treatment
The approach to goiter treatment is highly individualized, depending on the goiter’s size, its underlying cause, the presence of thyroid hormone dysfunction (hyperthyroidism or hypothyroidism), and the severity of symptoms. The primary goals of goiter treatment are to alleviate compressive symptoms, manage any hormonal imbalance, and, if necessary, address cosmetic concerns or malignancy. A comprehensive evaluation, including thyroid function tests (TSH, T3, T4), thyroid ultrasound, and sometimes fine-needle aspiration biopsy, guides the treatment decision-making process.
Medical Management of Goiter:
For goiters associated with thyroid dysfunction, medical therapy often focuses on correcting the hormone imbalance:
- Thyroid Hormone Replacement Therapy:
- Indication: This is the mainstay of treatment for hypothyroid goiters, particularly those caused by Hashimoto’s thyroiditis or iodine deficiency. It can also be used in euthyroid (normal thyroid function) goiters to attempt to shrink the gland or prevent further growth by suppressing TSH (Thyroid-Stimulating Hormone) secretion, which stimulates thyroid growth.
- Medication: Levothyroxine (synthetic T4) is the most commonly prescribed medication. The dose is carefully titrated to normalize TSH levels and, in some cases, to mildly suppress TSH to reduce goiter size.
- Effect: For hypothyroid goiters, levothyroxine therapy typically normalizes thyroid function and can lead to a reduction in goiter size in about 30-50% of cases. For euthyroid goiters, the success rate of shrinkage is variable, and long-term TSH suppression therapy carries risks like osteoporosis and atrial fibrillation.
- Antithyroid Medications:
- Indication: Used for hyperthyroid goiters, predominantly in Graves’ disease. These medications reduce the production of thyroid hormones.
- Medications: Methimazole and propylthiouracil (PTU) are common choices.
- Effect: They control hyperthyroid symptoms and can sometimes reduce goiter size by decreasing thyroid activity. Treatment is usually for 12-18 months, after which some patients may achieve remission.
- Iodine Supplementation:
- Indication: For goiters caused by iodine deficiency, particularly prevalent in certain geographical regions.
- Method: Supplementation through iodized salt, iodine-rich foods, or iodine supplements.
- Effect: Can prevent and, in early stages, sometimes reverse iodine deficiency goiters. However, excessive iodine intake can also cause or worsen thyroid dysfunction, so careful monitoring is necessary.
- Radioactive Iodine Therapy (RAI):
- Indication: Primarily for hyperthyroid goiters (e.g., Graves’ disease, toxic multinodular goiter, toxic adenoma) or large euthyroid goiters not responsive to other treatments.
- Method: The patient ingests a capsule or liquid containing radioactive iodine (I-131). The thyroid gland absorbs the iodine, and the radiation destroys overactive thyroid cells or shrinks the goiter over several weeks to months.
- Effect: Highly effective in treating hyperthyroidism and reducing goiter size. Often leads to lifelong hypothyroidism, requiring subsequent levothyroxine replacement.
Surgical Management of Goiter (Thyroidectomy):
Surgery is often considered when medical treatments are insufficient, or for specific indications:
- Indications for Thyroidectomy:
- Compressive Symptoms: When the goiter is large enough to cause significant difficulty swallowing, breathing, or voice changes due to pressure on the trachea, esophagus, or recurrent laryngeal nerve.
- Suspicion or Confirmation of Malignancy: If a thyroid nodule within the goiter is cancerous or highly suspicious for cancer based on biopsy results.
- Cosmetic Concerns: For very large or disfiguring goiters that significantly impact the patient’s appearance and quality of life, even if asymptomatic.
- Hyperthyroidism Unresponsive to Medical Therapy: For Graves’ disease or toxic multinodular goiter not controlled by antithyroid drugs or radioactive iodine, or when these treatments are contraindicated.
- Large Substernal Goiters: Goiters extending into the chest cavity can be difficult to manage medically and often require surgery due to the risk of compression.
- Types of Thyroidectomy:
- Total Thyroidectomy: Removal of the entire thyroid gland. This is often performed for cancer or very large multinodular goiters.
- Subtotal Thyroidectomy: Removal of most of the thyroid gland, leaving a small portion intact. Less common now, as recurrence rates can be higher.
- Lobectomy/Hemithyroidectomy: Removal of one lobe of the thyroid gland. Often chosen for unilateral nodules, smaller goiters, or low-risk cancers confined to one lobe.
- Post-surgical Considerations:
- Patients undergoing total or subtotal thyroidectomy will typically require lifelong thyroid hormone replacement therapy (levothyroxine) to prevent hypothyroidism.
- Potential surgical complications include temporary or permanent vocal cord paralysis (due to recurrent laryngeal nerve injury) and hypoparathyroidism (due to parathyroid gland injury, leading to low calcium levels).
Other Treatments and Considerations:
- Percutaneous Ethanol Injection (PEI): Used for autonomous functioning thyroid nodules or cystic nodules. Ethanol is injected into the nodule to destroy thyroid tissue.
- Radiofrequency Ablation (RFA) or Laser Ablation: Minimally invasive procedures used for benign solid thyroid nodules that cause compressive symptoms or cosmetic concerns, aiming to shrink the nodule without surgery.
- Observation: For small, asymptomatic, euthyroid goiters with no signs of malignancy, a “watch and wait” approach with regular monitoring (physical exams, ultrasound, thyroid function tests) may be appropriate.
- Dietary Considerations: Avoiding goitrogenic foods (e.g., raw cruciferous vegetables like cabbage, broccoli, kale) in large quantities might be advised in specific cases, especially if iodine intake is marginal, as these foods can interfere with thyroid hormone production.
Effective goiter treatment requires careful assessment of each patient’s unique presentation to choose the most appropriate and beneficial course of action for managing the goiter and its associated symptoms and conditions.